commentary Commentary
Commentary: HPV, the silent virus behind cervical cancer
Both early vaccination and early screening are key to eradicating this deadly virus and preventing cervical cancer, says NCIS’ Dr Ida Ismail-Pratt.
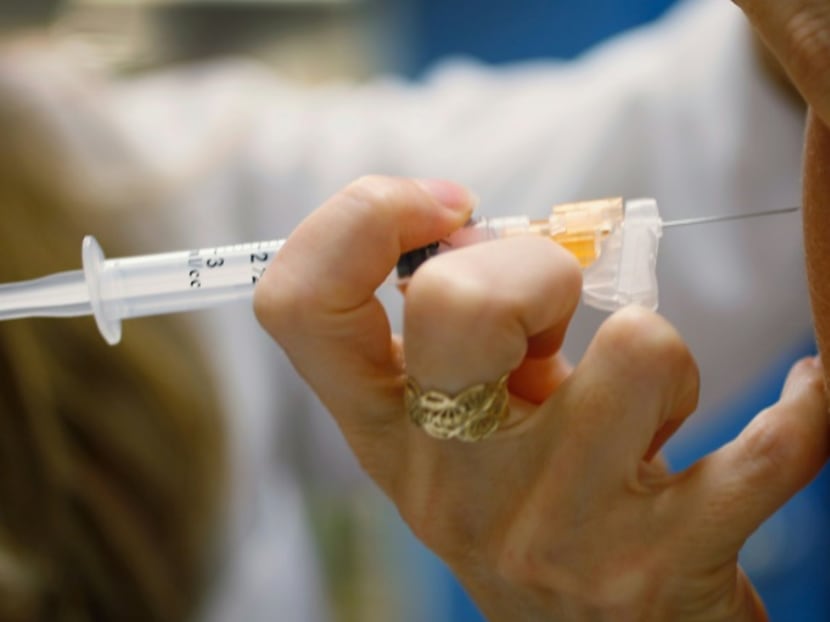
The human papillomavirus (HPV) vaccine has significantly reduced the incidence of cervical cancer (Photo: AFP/JOE RAEDLE)
SINGAPORE: Cervical cancer is one of the most commonly diagnosed cancer among women in Singapore. A worrying upward trend can be seen from the Singapore Cancer Registry report from 2011 to 2015.
A recent national survey by the Ministry of Health (MOH) also showed an increase in Singaporean women aged 30 and above diagnosed with late-stage cervical cancer, with no improvements in the uptake of cervical cancer screening among Singaporean women.
SILENT KILLER
Cervical cancer is a silent killer. It usually has no symptoms and when they do manifest, the cancer is already in its late stages.
Despite having an effective vaccine and screening tool, cervical cancer remains an epidemic worldwide, as the fourth most common gynaecological cancer globally, especially in developing countries.
While cervical cancer screening remains a pivotal player in the prevention of this disease, it has to work together with an effective Human Papillomavirus (HPV) vaccination programme.
MOVES TO STRENGTHEN CERVICAL CANCER SCREENING
In May 2018, the World Health Organisation’s (WHO) Director General Dr Tedros Adhanom Ghebreyesu called for the world to commit to a total eradication of cervical cancer.
In a timely move towards WHO’s goal, the MOH announced last Tuesday (Mar 5), the launch of the free HPV vaccination programme for Secondary 1 girls.
Singapore now stands alongside 50 other countries, such as Australia, Canada, Finland, Sweden, Malaysia and the United Kingdom in the global fight against cervical cancer.
Along with this announcement, MOH also introduced a more sensitive cervical cancer screening tool to detect pre-cancerous cervical lesions.
A HPV DNA test which needs to be carried out every five years will replace the pap smear test, which must be done every three years, as the new national cervical cancer screening protocol for women aged 30 and above.
PERSISTENCE OF HPV VIRUS
The HPV is a group of double-stranded DNA viruses extremely common worldwide and can be transmitted through skin contact including genital contact.
Women and men who are sexually active will be infected by this virus at some point in their life, though this does not mean that penetrative sex is a necessity for transmission.
There are more than 100 types of HPV. Fourteen are recognised to cause cancer. Among them are the HPV 16 and 18 types, which cause 70 per cent of cervical cancer and pre-cancerous lesions.
Acute infection including cancer-causing HPV infection does not increase the risk of developing cervical cancer. The issue lies in the persistence of the HPV infection.
THE HPV VACCINE AND CERVICAL CANCER PROTECTION
The HPV vaccine is a prophylactic vaccine. It protects the host against future cancer-causing HPV infections. It is a viral-like particle, and allows the vaccine to confer immunity without infecting the host.
It has a strong safety profile. The most reported adverse effect is pain where the injection occurs.
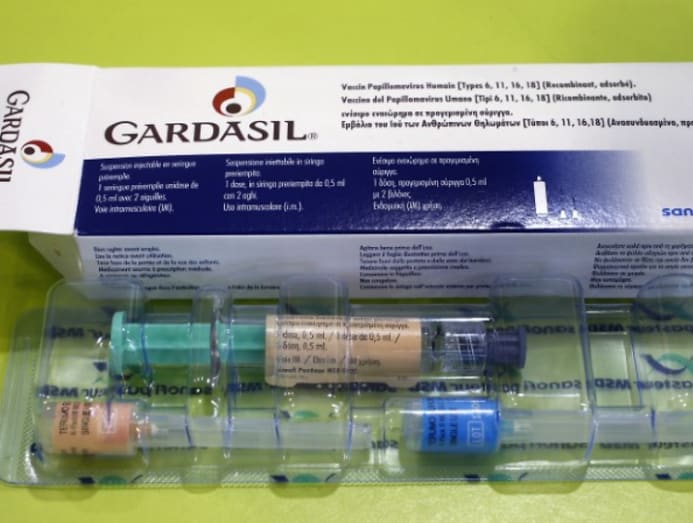
There are three HPV vaccines available worldwide; the bivalent, quadrivalent and nanovalent.
HPV vaccines are extremely effective in preventing the development of cervical cancer precursors, offering over 90 per cent protection. But none of these HPV vaccines will provide 100 per cent coverage.
Hence, regular cervical cancer screening must still be carried out because it can help to protect against other cancer-causing HPV infections not covered by the vaccine.
EARLY VACCINATION IS KEY
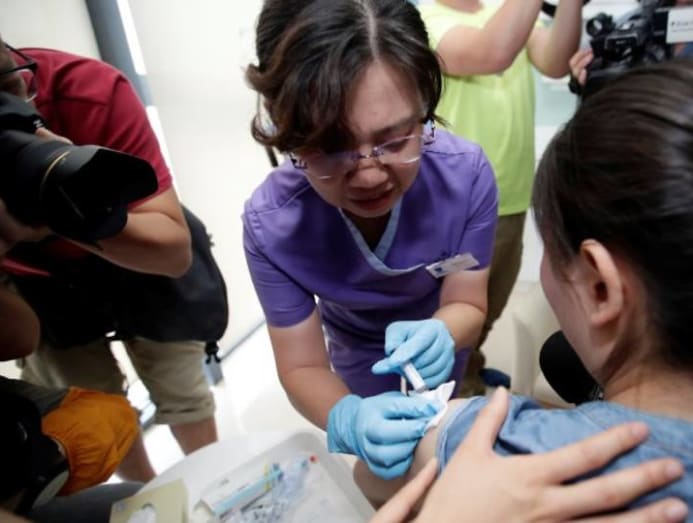
Still, adopting a school HPV vaccination programme is a crucial move towards the goal of eliminating cervical cancer. Protection is at its best if the vaccine is administered before a woman becomes sexually active.
In Singapore, the HPV vaccine is approved for use for young women aged 9 to 26 under the National Childhood Immunisation Schedule, with Medisave coverage of up to S$400.
Women up to the age of 45, who are already sexually active, with previous history of abnormal pap smear results or have been treated for pre-cancerous cervical lesions, may also benefit from the vaccine. In October 2018, the US Food and Drug Association (FDA) approved Gardasil 9 to be given to women up to 45.
HPV VACCINATION IN SINGAPOREAN MEN
There is also emerging evidence of a causal relationship between a tumour-causing HPV infection and the development of cancer in the anus, vulva, vagina, penis and oropharynx. HPV 16 is known to increase the risk of anal, penile and oropharyngeal cancers in men.
There is also emerging evidence regarding herd immunity and further reduction of cancer-related HPV infection in girls when the vaccination is also given to boys. Australia has adopted a gender-neutral school HPV vaccination programme and this has resulted in a significant reduction of their cervical cancer and HPV infection rates.
READ: HPV vaccine is safe, says cancer agency, slams 'unfounded rumours'
In Singapore, Gardasil and Gardasil 9 are licensed to be given to boys between 9 to 26 for protection against genital warts and anal pre-cancerous lesions.
EDUCATION AND AWARENESS
Cervical cancer is unique in that we not only now know its main causes but also its long natural history, which allows us to have an extremely effective prevention and screening tool to totally eradicate the disease in Singapore.
However, education and awareness are important aspects of our efforts.
It is not enough to just have these tools. As a nation we need to commit to using these tools as effectively as possible, to empower and protect our women from this terrible disease.
Dr Ida Ismail-Pratt is Consultant at National University Cancer Institute, Singapore’s Division of Gynaecologic Oncology.





