commentary Commentary
Commentary: At life's end, do we want to spend our last days in the hospital?
What we want out of care at the end of our lives is a good starting point for how we should design our palliative care system, argues Dr Cynthia Goh.
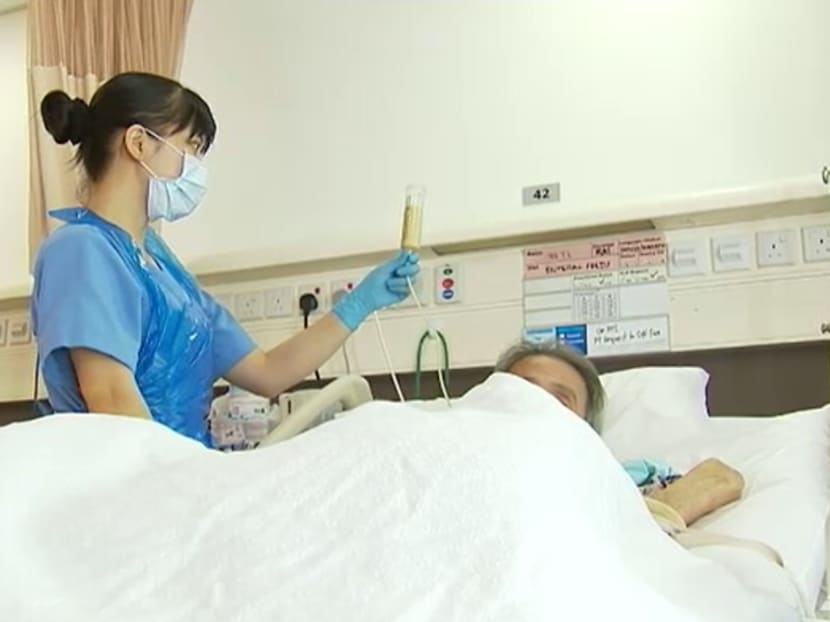
File photo of a nurse tending to a patient at a hospital in Singapore.
SINGAPORE: To prepare our healthcare system to deal with palliative care, increasing hospital or hospice beds or hiring more therapists or nurses are not the solutions.
The vast majority of us will face a life-threatening illness at some stage in our lives. When we do, what will be most important to us are how we want to be cared for during this illness and where we want to pass our days.
The illness may be a relatively short one, like cancer, and curable if diagnosed early, but often we might have to live with the disease for months, even years while undergoing cancer treatment. And each treatment session may be less effective, with more side effects than the one before, until we end up dying from the disease.
We may face other life-limiting illnesses, like heart failure or kidney failure. Treatment will sustain us for a while, again months or years. But there is no cure short of getting a new organ and that has its own problems, such as organ rejection and associated risks of infection.
Many of us will end up with long-drawn out illnesses that include dementia, stroke and various relapses. We will survive for many years but have to be content with disability.
We as a society need to discuss these issues and plan for different options that might be preferred by different people.
There is no one size that fits all.
GIVE PEOPLE CHOICES
For some, institutional care in a nursing home may be preferred. So we need to have institutions where people can thrive, not just subsist, where they can stay until they die and receive different levels of care according to their needs and as their conditions progress.
Many people say they want to be cared for and die in their own homes. That depends on whether there is anyone at home to care for us and what kind of support we can get at home.
Expansion of hospice home care services will obviously help. Skilled caregivers who are able to provide day-to-day care will also help.
Singapore is currently blessed with foreign domestic helpers who are affordable to many. But this may not necessarily continue in the future. Will our local people want to take up this work and even so, will the care remain affordable?
Most of us would not want to spend our last days in hospital, unless the medical interventions available there will actually prolong our lives and give us a life of reasonable quality. It is possible to spend a fortune on medical advances that may prolong life by a few weeks or months. This may be the wish of some and they should go for it, if they can afford it.
Others may not think the expense worthwhile, or find the burden of treatment too great. They should also be allowed their choice to spend their time and resources on different things.
So palliative care services should be designed to provide people with choices, whether it is outpatient care, home care, in-patient hospice care or care in nursing homes.
We should not leave it to voluntary welfare organisations to find solutions. For those not in need of government subsidies, or those not eligible for them, private enterprises should take up the challenge.
Retirement communities that cater to the healthy elderly, who can then transition to a higher level of care as one spouse becomes more dependent, or a person gets diagnosed with a life-limiting illness, is an idea. These may enable people to stay within their community and obtain needed medical and nursing input there, while enjoying familiar surroundings and the company of friends.
Different kinds of funding models can be experimented with, such as reverse mortgages or pooled risk.
CREATE SOLUTIONS OF OUR OWN
I think we need to think out of the box. We also need many heads to think and come up with new ideas. Different models of care and different kinds of services should be tried and tested out to see whether people like them, whether they can deliver what people want and whether they are sustainable.

I believe the consumer, and eventually this will include all of us, needs to play a much more active part in this discussion. I don’t think we should be doomed to whatever services evolve, but instead, create solutions of our own.
People should be encouraged to come up with new ideas. Funding should be made available to try out the better ideas, to see if they work and whether they can be scaled up.
A raft of ideas will provide options for different groups of people at different stages of their lives.
Yes, we shall have to train more therapists, more people in the healthcare sector and the care industry. But over-medicalisation of the situation is not desirable.
While people with life-threatening illnesses will need medical care, that is only one aspect of their care. They will also need a social life. They need to see their families, go out to eat, celebrate birthdays, or weddings, or anniversaries.
Some may need emotional support. Others might have financial worries. Still, others may have spiritual concerns or unfinished business.
Life is so much more than medical treatment.
So I think it is far too simplistic to think only about adding more hospital or hospice beds, which is what some people might have in mind. Understanding what people in different parts of our community want and trying out different ways of providing for choices is the way forward.
Associate Professor Cynthia Goh is a senior consultant at National Cancer Centre of Singapore’s Division of Palliative Medicine.
This is the third commentary in Channel NewsAsia's series exploring key issues and challenges facing patients with terminal illness and care at the end of life.





