Commentary: What if more terminally ill patients with COVID-19 want to die at home?
Helping vulnerable people with COVID-19 spend their last days at home might be worth the incremental risk, says local healthcare and bioethics experts Sumytra Menon, Anita Lim, Ryan Friets and Mathavi Senguttuvan.

An elderly man at the hospital. (Photo: iStock)
SINGAPORE: Mr Teo, a terminally ill 99-year-old who had contracted COVID-19, died at home in October.
Healthcare providers and family members had honoured his wish not to be hospitalised.
Still, should he still have been admitted to hospital since the Ministry of Health (MOH) recommends hospital care for those over 80 with COVID-19? To what extent should his wish to remain home be respected during the pandemic?
If this situation had arisen a year ago, Mr Teo would have been admitted to hospital for public health reasons, despite his wish to die at home.
But since then, home recovery has since become the default care arrangement for all in Singapore, except for some groups who may be clinically unsuitable or require closer monitoring.
In November, MOH also assured seniors that while the protocol is to convey those over 80 with COVID-19 for care in hospitals, “the practice is not rigid”. Those who prefer to be cared for in a familiar home environment would be supported to recover.
SHIFT IN HOW SINGAPORE THINKS ABOUT HOSPITALISATION
A year ago, Singapore was reporting single-digit number of daily COVID-19 cases. Protocols were aimed at controlling the spread of infection.
Hospitals were the main place where COVID-19 cases were sent for timely appropriate medical care, especially for seniors vulnerable to infection and severe disease. Information about the disease was still emerging, and vaccinations were not yet available in Singapore.
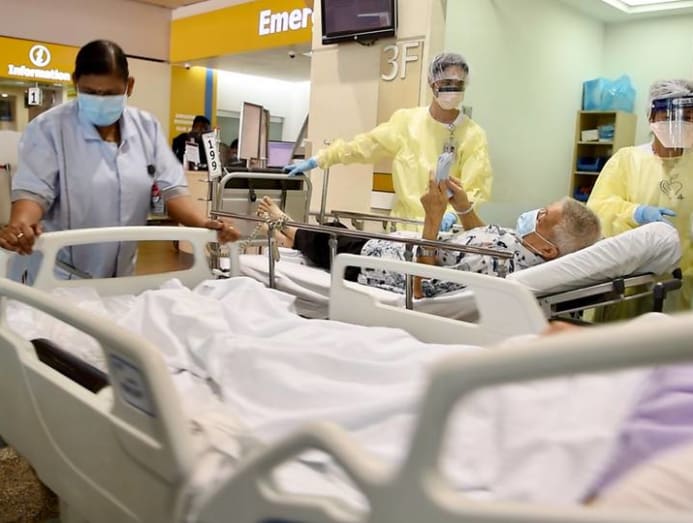
During this period, it would have been ethically permissible to override Mr Teo’s wish in the wider community interest to combat infection and minimise harm to others.
But as Singapore moves towards living with endemic COVID-19, our national response, including medical protocols, is evolving.
With 87 per cent of the population fully vaccinated in Singapore and almost 99 per cent who contract COVID-19 having asymptomatic or mild disease, mandatory hospitalisation is no longer justifiable for public health reasons nor sustainable for our healthcare system.
Unless they are immunocompromised or have serious underlying health issues and are deemed to have little chance of full recovery, home recovery would most likely be safe as evidence shows vaccination significantly reduces the risk of serious disease.
We also cannot continually defer non-urgent elective care to care for COVID-19 patients. Those who need hip or knee replacements, heart bypass or gall bladder surgeries may deteriorate while procedures are delayed.
In Singapore’s current situation, Mr Teo’s wish to remain at home should be respected. Being terminally ill, with a prognosis of short days to weeks, lends further weight to making his remaining time as comfortable as possible, in familiar surroundings, with his loved ones by his side.
HOME AS A PREFERRED COVID-19 RECOVERY SETTING
Individuals with COVID-19 may have many reasons to prefer home recovery, such as familiarity with the environment, access to home-cooked meals, and the comforting presence of family and caregivers.
Many are fully vaccinated. Infected individuals appear to be less likely to spread the virus to their loved ones at home, with household spread making up less than 10 per cent of cases, according to MOH.
This, of course, is also dependent on family members taking appropriate public health precautions such as using masks, conducting disinfection and isolating at home if in contact with the infected person.
Home-based care is also not new to many terminally ill patients. For them, spending their final days physically, mentally and emotionally isolated in a hospital may not be acceptable, even prior to the pandemic.
In particular, local researchers have shown that home palliative care during the pandemic is feasible with rigorous planning and workflows to protect patients, caregivers and health care workers.
After months at the frontline, hospitals are fighting COVID-19 surges. Listen to two doctors discuss how hospitals have been coping on CNA's Heart of the Matter:
When infections and clusters have risen in Singapore, we have at times implemented no-visitor policies in hospitals and nursing homes, with exceptions of up to five designated visitors for those nearing death.
The fluctuating nature of such policies could fuel fears of not being able to see family at all, which could in turn further the desire to die at home.
A DIGNIFIED DEATH IN THE TIME OF COVID-19
Globally, ethical and public health frameworks also lack adequate guidance for elderly patients managing COVID-19 illness at home.
Countries like the United States and United Kingdom saw their hospitals overwhelmed early in the pandemic. Faced with hard choices and the moral distress of rationing resources like ICU beds, the default course of action was to send more COVID-19 patients home to recover - or pass on, for the elderly with little prospect of recovery.
Singapore’s situation arises due to its stricter hospitalisation policy - part of our initial maximum suppression approach to buy time for the development of vaccines and treatments and avoid overwhelming our healthcare system.
We can look at countries like New Zealand who are pursuing a similar endemic approach to Singapore.
New Zealand enforces quarantine for COVID-19 cases, be it at home or in managed facilities, but their home recovery protocols are in a pilot stage and there is no guidance for those who wish to pass away at home.
Thus, public health considerations play a big role. If someone waiting to pass away remained at home, they would only be able to see other household members.
If Singapore has gradually restarted mass events and increased social gathering sizes, would it also be acceptable to allow visitors for those likely to pass away?
While this increases the risk of transmission from the infected person, this risk is outweighed by the benefits of allowing such people to die in the comfort of home with family and loved ones, and fulfilling their view of a dignified death.
This is because Singapore has already accepted that in the coming years most people will be infected with COVID-19, and a vast majority of vaccinated cases will likely experience minimal symptoms and recover fully.
Increasing visitation sizes for the terminally ill (both at home and in healthcare settings) would probably enhance the well-being of the terminally ill person and their family without much foreseeable impact on the overall public health situation. Government statistics show only 23 per cent of deaths in 2019 took place at home.
At the global level, the lack of adequate frameworks for dealing with patients wishing to die at home with COVID-19 represent a key opportunity for Singapore to be ahead of the curve in addressing the issue of deaths at home at a time when such guidance is severely lacking.
Health Minister Ong Ye Kung on Nov 8 said that the Government will support those who wish to die at home from COVID-19. This is certainly welcomed, but it remains to be seen how effective such changes will be in the face of other unforeseen events.
Respecting the elderly’s decision to spend their last days with loved ones is part of upholding their views of dignity and also beneficial from a public health perspective in alleviating an already strained health system by not hospitalising them.
As Singapore continues to advocate end-of-life planning, COVID-19 should not make us lose sight of what it means to die with dignity.
Sumytra Menon is Deputy Director at the Centre for Biomedical Ethics, NUS Yong Loo Lin School of Medicine. Anita Lim is Senior Consultant at the Division of Rheumatology, National University Hospital. Ryan Friets and Mathavi Senguttuvan are Research Associates at the Centre for Biomedical Ethics, NUS Yong Loo Lin School of Medicine. The opinions expressed are those of the writers.