What we know about Pfizer's Paxlovid, the first COVID-19 oral medicine approved for use in Singapore
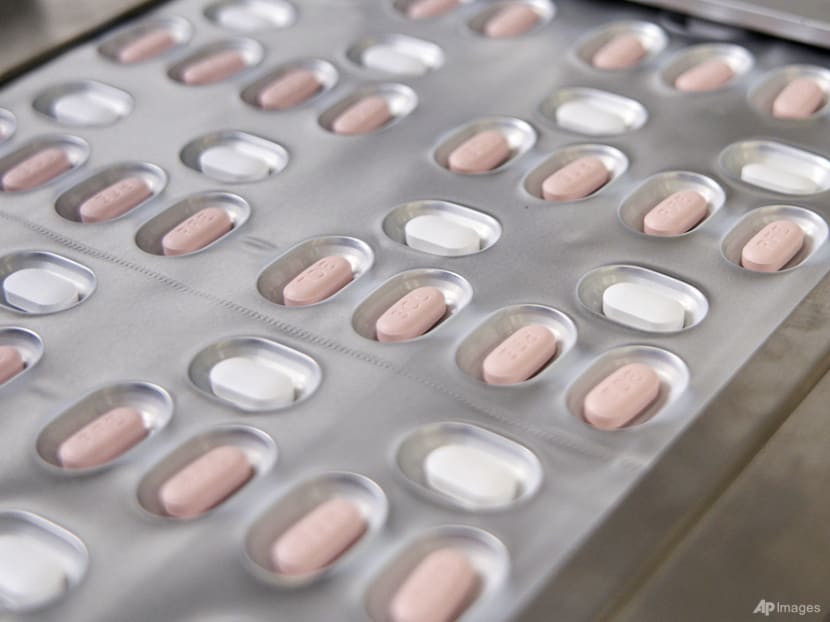
This image provided by Pfizer in October 2021 shows the company's COVID-19 Paxlovid pills. (Pfizer via AP)
SINGAPORE: The Health Sciences Authority (HSA) said on Thursday (Feb 3) it has approved the use of Pfizer's Paxlovid oral medicine to treat mild to moderate COVID-19 in adult patients who are at risk of severe disease.
The aim of this treatment is to reduce the risk of hospitalisation and death, HSA said.
The interim authorisation was granted under the Pandemic Special Access Route (PSAR), which also includes the Pfizer, Moderna and Sinovac COVID-19 vaccines.
Based on available clinical evidence, HSA said the benefits of Paxlovid outweigh the risks, pointing to a "favourable benefit-risk profile" for its use in the recommended patient group.
Paxlovid comprises two nirmatrelvir tablets and one ritonavir tablet, co-packaged for oral use. Nirmatrelvir is an antiviral medicine while ritonavir maintains the blood level of nirmatrelvir for antiviral efficacy.
Nirmatrelvir is designed to block the activity of an enzyme that the coronavirus needs to replicate, Pfizer said.
The Ministry of Health (MOH) confirmed that it is working with Pfizer to deliver the first batches of Paxlovid in February.
Here is what you need to know:
HOW EFFECTIVE IS IT?
Paxlovid has been found to reduce the risk of COVID-19 related hospitalisation or death by 88.9 per cent when treatment was given within three days of the onset of symptoms, according to a HSA review of available clinical data based on an ongoing Pfizer study.
When given within five days of the onset of symptoms, the medication reduces that risk by 87.8 per cent. The efficacy analysis included patients infected with the Delta variant.
HSA said in vitro data has also shown that Paxlovid is "active" against the prevailing variants of concern, including the Delta and Omicron variants.
More than 2,000 people aged 18 to 88 years old participated in the randomised, placebo-controlled study. All participants had mild to moderate COVID-19 and one or more risk factors for progression to severe disease.
A total of 1,039 participants were given Paxlovid and the rest - 1,046 people - received a placebo.
The results showed that 0.8 per cent of patients who received Paxlovid were hospitalised, compared to 6.3 per cent of those who received the placebo.
There were also no deaths in the Paxlovid group, compared to 12 deaths in the placebo group, HSA said.
The data has been submitted to a peer-reviewed publication and is expected to be published soon, Pfizer said.
Additional clinical trials are ongoing in adults at standard risk - which means low risk of hospitalisation or death - of progressing to severe illness, and in those who have been exposed to the virus through household contacts, it added.
WHO WILL BE ABLE TO TAKE IT?
Paxlovid will be prescribed to and prioritised for those at higher risk of severe COVID-19 illness, as directed by MOH.
The medicine should be taken twice a day for five days, HSA said. This means that patients will consume one course (two pink tablets of nirmatrelvir and one white tablet of ritonavir) in the morning and another course in evening.
Treatment should start as soon as possible after a COVID-19 diagnosis, within five days of the onset of COVID-19 symptoms, HSA said.
ARE THERE ANY SIDE EFFECTS?
HSA said the safety data showed that Paxlovid is "well-tolerated", adding that incidences of adverse events reported in the clinical study were "generally low".
Common adverse events reported were mild to moderate, such as altered sense of taste, diarrhoea, vomiting, hypertension, muscle pain and chills, said the authority.
Paxlovid might interact with various medications, such as medicines for irregular heart rate, migraine, and cholesterol, HSA said, adding that it could increase the amount of these medications in the blood and lead to "serious adverse events".
On the other hand, some medicines such as those for epileptic seizures could reduce the levels of Paxlovid, resulting in a loss of anti-viral efficacy, HSA said.
A prescribing doctor should carefully consider the potential for drug interactions before starting treatment, it stated.
WHERE ELSE IS PAXLOVID USED?
In December 2021, the US Food and Drug Administration (FDA) issued an emergency use authorisation for Paxlovid, although it warned that the treatment is not a substitute for vaccination in individuals for whom COVID-19 vaccination and a booster dose are recommended.
In January, the US doubled its order for Paxlovid to 20 million courses as it fights a record surge in COVID-19 cases.
For the first order of 10 million courses in November, the US government had said it would pay Pfizer US$5.29 billion.
"These pills will be delivered in the coming months and have been shown to dramatically decrease hospitalization and death from COVID-19," the White House said on Twitter.
On Jan 28, the European Commission granted a conditional marketing authorisation for Paxlovid, authorising it for use across the European Union (EU).
Italy, Germany and Belgium are among a handful of EU countries that have bought the drug.
In Asia, South Korea has also authorised Paxlovid for emergency use, and in January agreed to buy additional courses of the drug to cover 762,000 people.
WHAT'S NEXT FOR PAXLOVID?
As a requirement of interim authorisation, Pfizer will collect relevant safety data and monitor the use of Paxlovid.
HSA will also require Pfizer to continue submitting updated data from ongoing clinical studies to ensure the continued safety and efficacy of Paxlovid, including the drug's efficacy against prevailing variants.
Getting approval under PSAR means there is reasonable data suggesting that potential benefits outweigh known risks, and there are ongoing studies to generate continuing data to support an eventual transition to full registration of the products.
Interim authorisation of vaccines, medicines and medical devices under PSAR can be terminated by HSA at any time, such as when new data suggests that their benefits no longer outweigh their risks.
WHAT ABOUT OTHER COVID-19 ANTIVIRAL DRUGS?
The US FDA has also approved Merck's Molnupiravir antiviral drug for adults with COVID-19 who show early symptoms and face the highest risks of hospitalisation.
The approval, however, states that the drug should not be used during pregnancy as it could cause "fetal harm".
Merck’s pill is also under review in the EU, but is taking longer to approve because the company revised its trial data in November, saying the drug was significantly less effective than previously thought, Reuters reported.
In December, France cancelled its order for the drug following disappointing trial data.
In October last year, pharmaceutical company MSD announced that it has entered a supply and purchase agreement with Singapore to provide Molnupiravir, if it is authorised or approved.
Molnupiravir will be available for use after MSD submits their data to HSA and obtains authorisation for use in Singapore, said the Health Ministry, adding that the timeline for approval is dependent on the company’s submission of data to HSA.
MOH said it would continue to monitor the development of COVID-19 therapeutics and buy promising candidates to ensure Singapore has access to safe and effective COVID-19 treatments.






