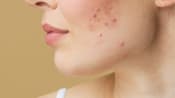
Here’s why misusing acne medications might make your body resistant to antibiotics
Are you prescribed creams, lotions and even pills when you see a doctor for acne? No, the clinic is not ripping you off – it has to do with preventing the development of antibiotic resistance.

(Photo: iStock/Boyloso)
As if suffering from acne isn’t bad enough for one's self-esteem, the wallet is also taking a hit when you’re paying for acne medications. Why can’t you just pay for some high-dose antibiotic pills, annihilate those acne-causing bacteria and call it a day?
That’s because you want to avoid developing antibiotic resistance. That same antibiotic that you take for acne could also be used for other infections such as pneumonia and sexually transmitted infections. And already, pneumonia and gonorrhoea are harder to beat with antibiotics, warned the World Health Organization.
Complications could also arise that can lengthen your hospital stay, increase medical care cost and more irreparably, “illnesses caused by antibiotic-resistant bacteria are harder or impossible to treat, and can lead to disability and death”, according to Healthhub.
But what does antibiotic resistance have to do with the many tubes of creams you receive for your acne? And how can you prevent the development of antibiotic resistance?

WHAT IS ACNE REALLY?
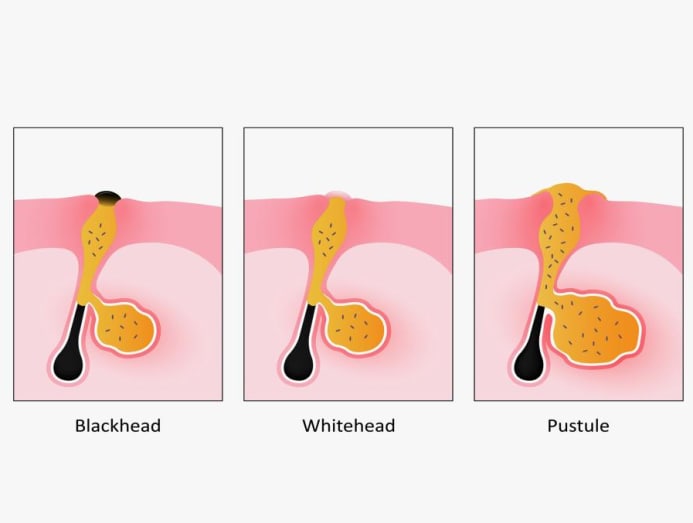
The comedones or small bumps that give rise to acne (or acne vulgaris in medical terms) are hair follicles choked with excess sebum and dead skin cells, said Dr Eileen Tan, a dermatologist with Mount Elizabeth Novena Hospital, leading to what you know as blackheads or whiteheads.
The only difference between a blackhead and whitehead is whether your skin closes or remains open over the pore. If the pore is open, the sebum is exposed and gets oxidised, resulting in a blackhead. If it is closed, it becomes a whitehead.
As for the culprit that causes those red, swollen and painful blemishes, that would be the bacterium Propionibacterium acnes (P. acnes for short). This skin bacteria feed on plugs of sebum and dead skin in the hair follicles, and trigger your immune system to react by creating inflammed and pus-filled pustules.
WHY ARE ANTIBIOTICS LOSING THE FIGHT? HOW BAD IS IT?
Antibiotics usually do the job of clearing the acne up – and the dosage doesn’t have to be high, according to Associate Professor Adam Friedman from George Washington University.
“Research has shown that the desired anti-inflammatory effects can be achieved at sub-antibacterial dosing. This means that the needed dose is so low that it can’t kill good bacteria or challenge pathogenic bacteria to become resistant," he wrote in The Conversation.
However, no thanks to keeping patients longer on antibiotics and using higher-than-needed doses – at least in the United States – P. acnes has developed resistance to some antibiotics, said Assoc Prof Friedman.
The overuse of antibiotics has also led to more harmful skin bacteria such as Staphlycoccus aureus and Streptococcus becoming resistant, he wrote.
In the United Kingdom, “antibiotic-resistant strains of P. acnes have increased steadily since the 1970s and are now found in more than 50 per cent of cases there”, said Dr Tan.
In Singapore, P. acnes appears to have also developed some resistance, according to research on more than 1,000 adolescents in Singapore. In this 2007 study, 26 subjects or nearly 15 per cent were found to have antibiotic-resistant strains of P. acnes.
What’s worrying is that 58 per cent of the teens, who carried antibiotic-resistant strains of P. acnes, did not have a history of antibiotic use for acne. The authors concluded that there is a need for the “accurate education on acne and its appropriate treatment” to stem the further development of more resistant P. acnes strains.
WHEN ARE ORAL OR TOPICAL ANTIBIOTICS USED TO TREAT ACNE?
It depends on the acne’s severity, said Dr Ang Sue May, a consultant with National Skin Centre. This can be ascertained using the Global Acne Grading System. For mild to moderate acne, topical antibiotics such as clindamycin and erythromycin can be prescribed, she said.
For oral antibiotics, noted Dr Ang, they are usually prescribed for “moderate to severe acne that does not respond to other treatments or for inflammatory acne that does not respond to topical antibiotics”.
P. ACNES OR C. ACNES?
When it comes to the acne-causing bacteria, you may have come across the name "Cutibacterium acnes" (C. acnes) instead of "Propionibacterium acnes" (P. acnes) in some research articles.
That's because the Propionibacteriaceae family that the acne bacteria belongs to is very diverse (it also includes bacteria that live in cheese, dairy products and cattle rumen). Scientists recently broke it up into three subgroups – one of which is Cutibacterium and it specifically refers to the strain of bacteria that inhabits human skin.
“Doxycycline, tetracycline and erythromycin are recommended as first-line oral antibiotics,” said Dr Ang. You may be given minocycline only when those don’t work as the former has “more severe adverse events”, she said.
As you step up to more potent antibiotics, more serious effects usually accompany them, such as cotrimoxazole, which can potentially cause Stevens-Johnson syndrome or toxic epidermal necrolysis, said Dr Ang.
HOW DO WE TELL IF OUR SKIN HAS DEVELOPED A RESISTANCE TO ANTIBIOTICS?
“It is the acne bacteria that develop resistance to antibiotics,” said Dr Moosa Aminath Shiwaza, an associate consultant with SingHealth Polyclinics. “It’s not a skin problem therefore, the skin will not show any signs.”
But if your acne shows “a reduced response, no response or a relapse”, said Dr Ang, there is a chance that the bacteria have developed a resistance to the antibiotic you’re on. This is especially so after using a topical antibiotic after four to eight weeks, said Dr Tan.
For oral antibiotics, Dr Tan said that "resistance to tetracycline is less common than to erythromycin and is least with minocycline."

On the whole, antibiotic resistance can occur in “30 per cent to 60 per cent of cases, depending on the regions and countries”, said Dr Ang.
In Singapore, Dr Moosa said that “it is not possible for us to know how often we see patients with antibiotic resistance in acne treatment” as testing for bacterial resistance is not done routinely. “Those tests are not necessary for initiating or switching therapy.”
DOES THE RESISTANCE CAUSED BY THE MISUSE OF ANTIBIOTICS FOR ACNE ALSO AFFECT GENERAL HEALTH?
If it’s an antibiotic cream, the “damage” is confined to the skin of the treated area, said Dr Ang. For oral antibiotics, they can “lead to antibiotic resistance” throughout your body, she said.
According to Dr Moosa, “bacteria develop antibiotic resistance to specific antibiotics, not all antibiotics”. “This means other antibiotics can still work against the bacteria.” Still, that doesn’t mean it’s okay to misuse antibiotics such as sharing them with family members, using them for viral infections or not completing the course as intended.

How long the antibiotic resistance lasts depends on how extensive the misuse of antibiotics is. “Evolution is the cause of the resistance,” noted researchers from Netherlands Organization for Scientific Research in Science Daily.
"This resistance should disappear again as resistant (bacteria) grow less well in an environment without the substance they are resistant to and are therefore, outstripped by their faster-growing non-resistant counterparts. Yet, some variants remain permanently resistant.”
BUT WHY DO I GET SO MANY MEDICATIONS JUST FOR ACNE?
Doctors generally avoid prescribing oral and topical antibiotics together to prevent the overuse of these medicines. And when an antibiotic does get prescribed, it is not about hitting the bacteria as hard as possible with the highest possible dose.
Rather, it is about using a low but sufficient dose to take out the acne bacteria without upsetting your body's microbiome – and more importantly, prevent the development of antibiotic resistance, according to Assoc Prof Friedman.
To “make the treatment more effective, reduce antibiotic resistance and to maintain the results after the course is over”, other topical agents such as benzoyl peroxide are usually prescribed alongside to reduce the number of bacteria and provide an anti-inflammatory effect, said Dr Ang. This is why you'll usually receive other tubes or tubs in your little plastic bag when you see a doctor for acne.

Topical retinoids (such as tretinoin and adapalene) may be deployed to remove dead skin cells from the surface of the skin, which helps prevent the hair follicles from getting clogged, she said.
Other topical agents such as salicylic acid or azelaic acid may also be used alongside antibiotics. The latter, said Dr Ang, is a good alternative if you can’t tolerate the “irritating or painful” side effects of benzoyl peroxide or retinoids.
“A minimum of six to eight weeks of treatment is recommended,” said Dr Tan, when it comes to using antibiotics (oral or topical) and other topical agents.
When oral antibiotics are involved – along with a topical retinoid, benzoyl peroxide or other combination – they should ideally be prescribed for no longer than three months, said Dr Ang.