Life with chronic kidney disease since 18: He was told he had 7 years to live – he’s now in his active 50s
Job Loei, 57, recalled the shock when he was diagnosed with the medical condition at a young age. But he has since spent 28 years and counting on dialysis and loving life. This is his story.

Kidney patient Job Loei, 57, paragliding in Switzerland before the pandemic (left) and in-between workouts in his office gym. (Photos: Job Loei)
Imagine being so thirsty, you wish you could drink the moisture right off the humidity in Singapore. But you can’t – not because it is impossible to do so, but because you’ve already hit your fluid quota, which can be as little as 500ml a day. That quota includes not only plain water but any food or drink such as coffee, tea, juice, soup, gravy, porridge and even ice cream that contributes to your fluid intake at room temperature.
Such is the constant struggle for chronic kidney disease (CKD) patients who are on dialysis. And for good reason: They pass very little or no urine at all as a result of their reduced kidney function. This means that fluid build-up in the body can lead to issues such as heart problems or fluids in the lungs if they don’t control their fluid intake.
And while you may have heard of dialysis, you may not be aware that some of these patients have to have an arteriovenous or AV fistula surgically created beforehand. It involves stitching an artery and vein in the forearm together to create a reinforced access point for the two dialysis needles. This reinforcement is crucial because, unlike a one-off blood withdrawal during a health check or blood donation drive, the vein has to be sturdy enough for repeated use.
Those are the experiences that Job Loei, a CKD patient of 39 years, is all too familiar with. “Kidney patients can be very conscious of our fistulas,” Loei shared when asked about his. “An experience I had on the MRT was with two youths who reacted visibly shocked when they saw my arm, like, why does it look like that?” he said of the thick, keloid-like protrusion running down the length of his left forearm.
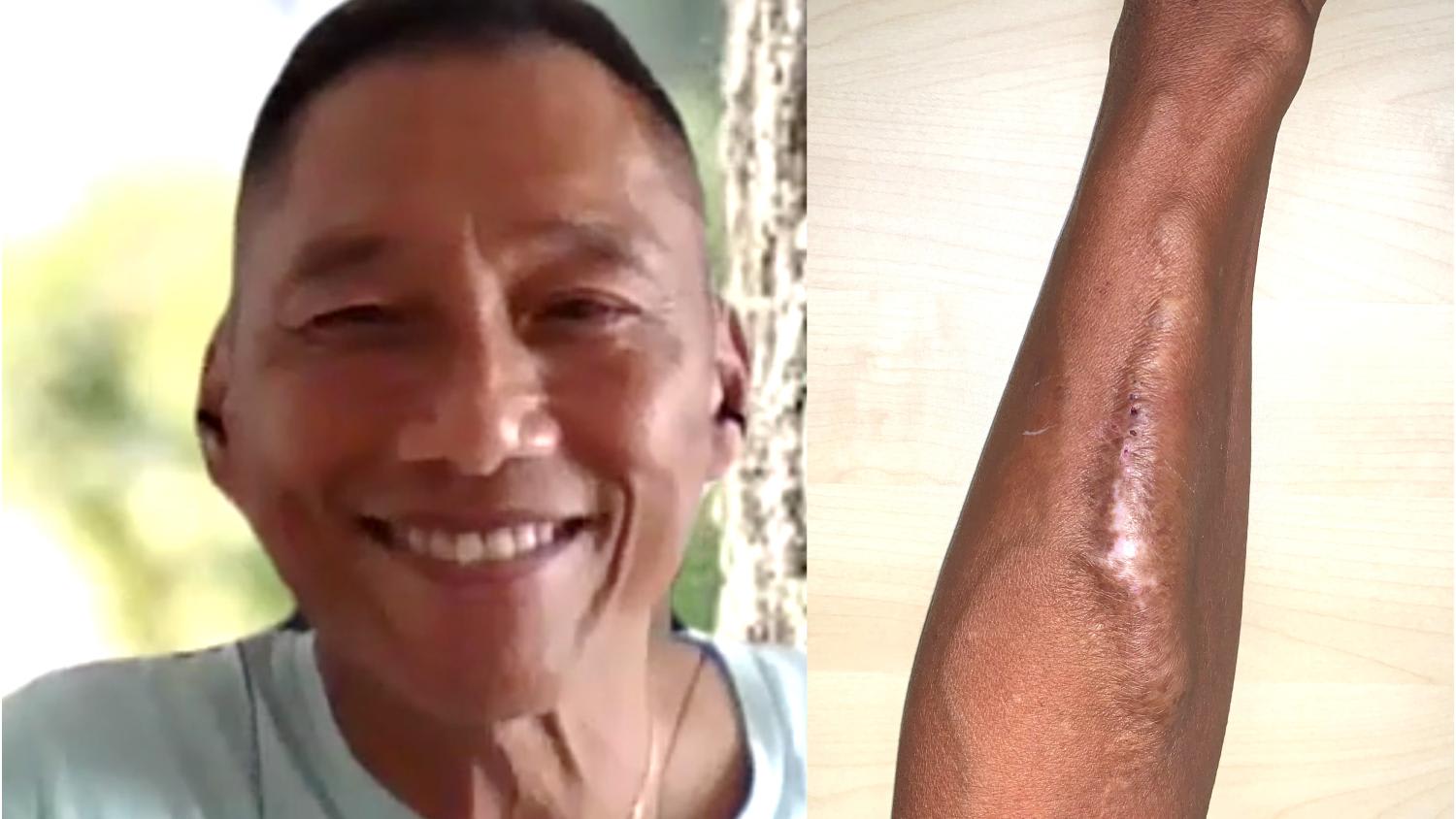
But lest you think the 57-year-old, who works as a manager at a non-profit organisation, is a pale, frail recluse, you’d be in for a surprise. In the online interview with CNA Lifestyle, it was evident that his deep tan and trim figure could pass him off as an active 40-something.
Loei’s fit appearance isn’t the only thing that surprises most people. At an unusually young age of 18, he was diagnosed with chronic glomerulonephritis in both kidneys, which refers to the inflammation of the organs' tiny filters. It came as a shock to him as he was a school athlete then and didn’t have a family history of kidney disease – or any prior medical history for that matter.
“It was one of the most unforgettable experiences in my life,” said Loei of the results he received from his medical check-up for national service. “I was naive and didn’t realise that it was a serious condition. I thought it could be treated.”
The avid runner enlisted nonetheless but life was an emotional yoyo from then on. There were frequent hospital visits to make and urine samples to submit. “I’d get panic attacks and feel nauseous from the fear of hearing more bad news. And the anxiety would last a few days after each appointment,” he said.
“But after a while, my life would reset to normal. It’s how we are as humans, right? We become accepting of our situation and go back to our lives. But the anxiety would peak again at my next appointment. That was my life then.”
CHRONIC KIDNEY DISEASE IN YOUNG PEOPLE
Chronic kidney disease (CKD) is when the kidneys are not able to function normally, which leads to the body’s inability to remove waste and water effectively, said Dr Alvin Ng, a senior consultant nephrologist at Mount Elizabeth Novena Hospital’s The Kidney & Transplant Practice.
“CKD is irreversible as the kidneys would already have undergone damage before the disease is detected,” he said. “The severity of kidney disease can range from mild to moderate and severe kidney impairment.”
The disease's prevalence increases with age with nearly 30 per cent of CKD patients coming from the 70-to-74 age group, according to Singapore's National Population Health Survey 2020. Older patients also typically suffer from diabetes, hypertension or have a family history of kidney disease.
In contrast, the causes of CKD in young people are usually "urine blockages, reflux nephropathy (the backflow of urine into the kidney), birth defects or nephrotic syndrome (your body passes out too much albumin, a protein that helps your body to get rid of excess fluid)”, said Dr Ng.
DON'T EXPECT TO LIVE LONGER THAN SEVEN YEARS
It was in his 20s when Loei started to feel the symptoms of kidney failure, which can include nausea, vomiting, loss of appetite, fatigue, sleep problems, urinating more or less, decreased mental sharpness and/or muscle cramps.
“Kidney disease is such that you don’t feel any symptoms in the beginning. I was at age 24 or 25 when my symptoms started to surface,” he said. In addition, he developed very painful gout and mild hypertension as well.
That was also the time he started dating and he wanted to know where his future was heading. How long could he expect to live? Is his condition hereditary? Would his offspring develop kidney disease, too? “My girlfriend knew about my health and was accepting of it,” he said. Her parents? Not so.
“I was told that my kidneys were damaged but I had no idea to what extent,” he recalled. “The doctor did not explain to me my CKD stage, like if you’re Stage 3, you can slow down the kidney deterioration by watching your diet,” he said. Instead, the young man was told: Don’t expect to live longer than seven years.
“It was difficult in the beginning. I visited her parents and I was honest with them. I am thankful that they eventually gave us their blessings. She’s now my wife,” he said, smiling.
At age 27, nine years after he was first diagnosed, Loei’s doctor brought up the need for an AV fistula procedure before he could undergo haemodialysis. “I didn’t know about other options such as peritoneal dialysis, which didn’t require a fistula. At that time, there weren’t any renal coordinators or medical social workers like what they do now in hospitals,” he said. “I had no such provisions. I had to believe what the doctor told me”.
It was only a year after his fistula procedure that Loei began dialysis. (He didn't require dialysis immediately and moreover, a fistula takes about six to 12 weeks to mature before it can be used.) “The first thing that came into my mind was, without this machine, I could die. This was it. I would be stuck to this chair for the rest of my life.
“That was the day I thought to myself: I had to give up my dreams. I love to travel. I wanted to work in the air force or become an air steward. But it was no more. I couldn’t even dare to imagine the chance to travel,” he said.
COMING OUT OF THE DARK
Dark days for the father of one followed and he became “depressed and fearful”. “My son was about two years old when I started my dialysis,” he said, describing how his boy would shy away from him when he saw the tubes of blood.
His wife and son would sometimes accompany him on those four-hour sessions at the dialysis centre. “My wife felt very helpless and didn’t know what to do. My parents started blaming themselves for how my health turned out,” he said.
A healthy person's kidneys filter about 90ml to 120ml of blood per minute. Patients with kidney failure filter less than 15ml of blood per minute.
Loei couldn’t let the negativity inside him affect his loved ones after seeing the change in them. “That was the turning point. I had to be strong, at least for my boy. I probably wouldn’t live very long but even so, I could still give my son a good childhood. So I decided to change.”
Two of the milestones he’d achieved in the dialysis chair was earning his master's degrees: One in social work and the other in counselling from Monash University in Australia. “I think I’ve spent over 4,000 days on dialysis so far,” he said, based on the thrice weekly sessions he’d been going for. “I myself am overwhelmed. But I’m thankful I have the chance to live this long.”
DIFFERENT TYPES OF DIALYSIS
Haemodialysis: The dialysis machine removes blood from the patient, cleanses it of toxins, extra salt and fluids, then returns the cleaned blood to the patient. It also helps patients maintain balance in their potassium, sodium and chloride levels as well as keeps blood pressure under control.
Peritoneal dialysis: A fluid is introduced into the patient’s abdomen through a permanent tube placed in the peritoneal cavity. The fluid circulates through the abdomen to draw impurities from the surrounding blood vessels in the abdominal cavity and is then drained from the body. There are two types of peritoneal dialysis: Continuous ambulatory peritoneal dialysis (CAPD) and automated peritoneal dialysis (APD).
Haemodiafiltration: The process is similar to haemodialysis but it can also remove more middle-molecular-weight solutes. The advantages of this treatment are better control of hypertension and hyperhydration.
TAKING CHARGE
Loei’s zest for life is evident in his pictures. A gleeful, pre-pandemic photo of him paragliding in Switzerland, a fitspo selfie captured in the office gym… they all point to a man who is making lemonade with the lemons that life has given him.
Take his wish to see the southern lights, for instance. The nearest country for that is New Zealand but “it would have been impractical for me to travel long hours to get to the dialysis centre there”, he explained. “And I’m not comfortable to perform my own dialysis on a portable machine.”
So he did the next best thing – and upgraded to a trip to Switzerland instead. “There was paragliding and it was something I’ve always wanted to try. I am very thankful that my wife told me to travel before I reached 55,” he laughed.
THE SILENT KILLER
There are currently more than 8,500 dialysis patients in Singapore, according to the Singapore Renal Registry Annual Report 2020. About 5.7 new patients are diagnosed daily.
However, 95 per cent of people with mild chronic kidney disease (CKD) do not know they have it. Almost half of people with severe CKD are completely unaware they are ill.
“In most cases of progressive kidney disease, the body can adjust to the build-up of toxins and the patient will only feel unwell once their kidney function falls below 15 per cent,” said Dr Alvin Ng, a senior consultant nephrologist at Mount Elizabeth Novena Hospital’s The Kidney & Transplant Practice.
"It is recommended for anyone from age 30 to have a kidney health check," said Dr Ng. If the person has risk factors such as diabetes mellitus, high blood pressure, a family history of kidney disease or is a smoker, they should check earlier."
CKD can be detected with a urine and blood test. Most times, an ultrasound scan of the kidneys is also done, he added.
He was also among the first kidney patients to go for the COVID-19 jabs, including the booster shot. “I seized the opportunity. Some patients are concerned about the side effects. I was aware of them and I’ve read about people dying from the side effects. But I believe the shots are for my own protection. That’s why knowledge is very important. You need it to make informed decisions.”
Loei’s mantra "knowledge is power" hasn’t gone unnoticed at work and among hospital staff; he is often asked to counsel kidney patients. “Just before the pandemic, I was asked to talk to a 19-year-old, who was about to enlist in the army and was diagnosed with kidney disease,” he shared. “He had to undergo certain procedures that totally freaked him out. It reminded me of myself.
“Immediately after getting the call, I went down to the hospital. He was crying when I got to the ward,” he said. “Some of the procedures were unpleasant. I told him, ‘You don’t have to go through them. You have the right not to. I believe the doctor can find other ways and means to help’. I was able to calm him down.”

ANOTHER HEALTH SCARE
Loei’s positive attitude has stood him in good stead, even when he had another health scare after 10 years of dialysis. “I was diagnosed with a pulmonary valve leak and I needed a bypass. I was scared and sad. But I had 10 years of experience dealing with my health, so I knew what I can do to help myself.”
So, Loei did something most patients wouldn't think of doing: He took up jogging – and was able to eventually forgo the bypass surgery. “The beginning was difficult as I hadn’t been exercising for a long time. It took a lot of willpower and discipline. Finally, I was able to jog three or four times a week; each time covering 10km. And I jogged regularly for many years.”
These days, he’ll wake up at 4.45am to jog at Bedok Reservoir on his non-dialysis days. “I’ll finish with stretching and a shower at around 7am and start my work at home.”
Even though he is taking things slower now (he covers 6km instead), his fitness routine is still enough to put some individuals half his age to shame. When he’s not jogging, he’ll spend three to four hours riding his foldable bicycle from Tampines to Pasir Ris Park and sometimes, all the way to East Coast Park.

EXERCISE IS KEY
How does Loei cope with exercise-induced thirst when, as a CKD patient, his fluid intake has to be severely limited? “Because I lose fluid through perspiration, I am allowed more water than the average patient,” he explained, noting that he drinks about one litre of water a day when he exercises. It is a stark contrast to the other patients, who may only be allowed 500ml or 800ml of fluid a day. “That’s why I always encourage patients to exercise,” he said.
Being active has also reaped him other health benefits. For one, he no longer has to take medicine for hypertension. “Some patients have 10 different types of medicine. At this point, I only take about four or five pills a day, including my cholesterol meds and multivitamins.”
Certainly, a strict diet is crucial to kidney patients but that hasn’t stopped Loei from eating out. “I eat out most of the time. I usually opt for economy rice because I can control what I eat better. And because of my exercise, I no longer have hypertension, so salty food has less of an impact on me.”
However, he still adheres to food that is low in phosphorus, potassium, sodium and oil. “If you don’t control your phosphate intake, it will affect your bone health. If you eat too much high-potassium fruits or vegetables, for example, it will impact your heart,” he explained.
Loei's secret to looking and feeling good is simple. "Because of how I care for myself, I don’t look like a patient. And sometimes, I forget about my condition," he said.
His advice for fellow kidney patients? "Your body needs treatment but you also need to equip yourself with knowledge. You need to control your water intake, eat properly, take your medication, stay compliant with your treatment and exercise. More importantly, you have to stay positive."





