Why snoring loudly could be linked to heart disease, hypertension or worse
Obstructive sleep apnoea is a common condition among Singaporeans. Experts from SingHealth Polyclinics explain how to deal with it – including doing mouth exercises like ‘tongue tai chi’.

(Photo: Freepik/katemangostar)
When it comes to snoring, it’s never good news for your bed partner and yourself. Apart from the nightly noise that keeps everyone around you awake, snoring is not a sign you’re sleeping deeply and well either.
In fact, if your partner complains that you not only snore loudly but also sound like you’re gasping or choking in your sleep, you may have obstructive sleep apnoea (OSA).
Worryingly enough, fighting for air isn’t that far off from what’s really happening to you.
That’s because the muscles at the back of your throat relax and collapse during sleep, even while you’re trying to breathe. This closes the airway and triggers a drop in the oxygen supply to your organs, especially the brain.
READ: The benefits of napping – and how to snooze without affecting your sleep at night
To keep you alive, your body goes into self-preservation mode and forces you to wake up briefly – but long enough – for you to open up the airway again, explained Dr Tan Teck Shi, the clinical lead for a respiratory workshop with SingHealth Polyclinics.
This is why OSA patients snore louder and louder like a crescendo. Then, the snoring stops and is followed by a gasp that can sound like a snort. This “symphony” repeats itself all over again throughout the night, except it’s no music to your partner’s ears.
OSA is a common condition seen among Singaporeans, as it turns out. According to Dr Tan, over 1,000 patients visit SingHealth Polyclinics every month, and a telltale sign they have it: Snoring.

WHAT CAUSES OSA AND WHAT ARE THE COMPLICATIONS?
A proper night’s rest is out of the question, owing to your body’s many wake-up calls. You wake up tired. You have morning headaches and weight gain despite watching your diet.
But that’s not all. “The danger of sleep apnoea is the combination of disturbed sleep and oxygen starvation, which may lead to hypertension, heart disease, heart failure, abnormal heart rhythms, or even stroke,” said Dr Tan.
READ: Are you grinding your teeth? You could be stressed or have a sleeping disorder
“Mood disorders, drowsiness, depression and memory problems may also surface. Other associated conditions include the increased risk of getting diabetes and its complications as well as sexual dysfunction.”
Age is a common reason why you’re more prone to OSA and snoring the older you get. “The throat muscles and tongue tend to relax more during sleep and will fall backwards as one ages.
This causes a narrowing of the throat, which results in the vibration sound of snoring, especially during inhalation,” said Dr Tan.
Being overweight, which often comes with age, further compounds the problem as it leads to poor muscle tone, and increases the tissue around the neck and throat.

OSA can also be attributed to congenital issues, such as a narrower air passage in the nostrils caused by a deviated septum (the cartilage separating the nostrils).
“People who are born with a recessed chin, small jaw or a large overbite can have a narrowed nose and throat passage, which may cause snoring to occur,” said Dr Tan.
Soft tissue growths on the lining of the nasal passages, sinuses, throat or tonsils, are other factors, he added.
READ: Can’t sleep at night, dozing off in the day – it could point to bigger health issues
Medical reasons are another consideration. For instance, low thyroid hormones or hypothyroidism can cause muscular weakness, and fat tissue to be deposited around the upper airway that may cause the person to snore.
If you have an allergy or a cold, that and the medications you take to counter the sniffles, can cause snoring. “Medication can act as a strong muscle relaxant that causes the area around the throat and airway to slacken during sleep, resulting in snoring,” said Dr Tan.
HOW DO YOU GET DIAGNOSED?
Consult your family doctor if you suspect you have OSA. If required, he will then refer you to the relevant specialist.
To verify if you suffer from OSA, you may be put through the Home Sleep Test. Dr Tan explains that it entails wearing a portable monitoring device that is similar to a wristwatch.

A probe is also worn on a finger to monitor your oxygen levels, pulse rate and peripheral arterial tone, along with a chest sensor to measure your body movements and snoring level.
“The patient is required to attach the device at home while sleeping through the night. It typically takes only one night to complete the test,” he said.
EXERCISES TO MINIMISE SNORING
The diagnosis is out and you do have OSA. What’s next? One simple way is to sleep on your side. Patients tend to snore less in this position than sleeping on their back, said Dr Tan.
Like the muscles in your body, the muscles controlling your tongue and those at the back of the throat can also be strengthened, said Dr Ruebini Anandarajan, the head of dental services at SingHealth Polyclinics.
There are upper airway exercises you can perform, though she advised that it is best to do them under the supervision of your sleep specialist.
Here are some basic examples you can try at least once a day, said Dr Anandarajan:
Tongue curls. Open your mouth wide and stretch your tongue down as far as possible towards your chin. Hold for at least 5 seconds. Repeat 5 times.
Tongue press. Suck your tongue upwards against the hard palate. Continue sucking while opening your mouth wide. Repeat up to 5 times.
Tongue tai chi. Poke your tongue against your left and right cheek alternately. You can increase the resistance against the tongue by pushing your cheek against the tongue with your fingers. Hold for 5 seconds. Repeat up to 5 times on each side.
Swallow saliva. Hold your tongue between your lips and swallow your saliva. Repeat up to 5 times.
Mouth blowing. Inhale through your nose and exhale through your mouth while keeping your lips pressed together like blowing an imaginary balloon. Blow for 5 seconds. You can repeat up to 10 times.
WHAT ARE THE TREATMENT OPTIONS?
If you’re after the standard and “highly effective” way of managing OSA, it’s to use the Continuous Positive Airway Pressure (CPAP) machine, which you can buy or rent, said Dr Tan.
It pumps air into your airway to keep it from collapsing while you sleep. “The noise level of the machine is typically less than 30 dB, which can be compared to the sound of a whisper.”
Furthermore, data about your response to the treatment can be stored on a memory card or directly to an app on your mobile phone or computer, he added.
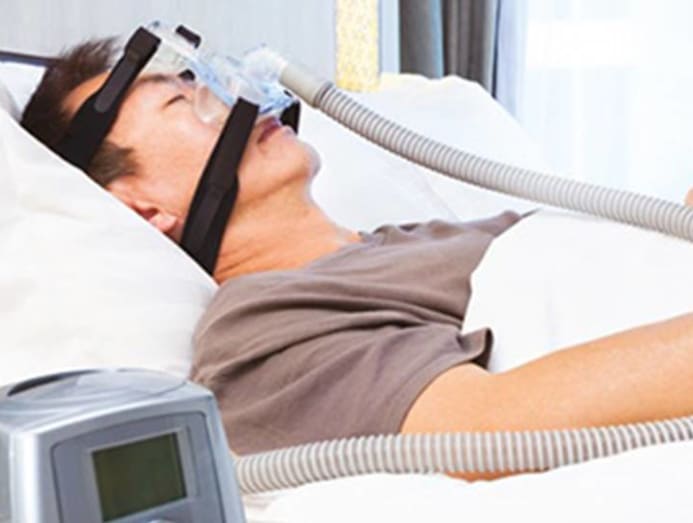
There are some downsides, though. The air is pumped to the nose through a flexible tubing connected to the shoebox-sized CPAP machine, which means you have to wear a mask during sleep.
Not good news if you toss and turn a lot at night – or you don’t like wearing something over your face while you sleep.
Another way is to use oral appliances prescribed by a dentist, who specialises in sleep apnoea management, said Dr Anandarajan.
“An oral appliance for sleep apnoea is worn during sleep. It works by shifting the lower jaw (mandible) slightly forward to open up the airway.
“As the shift can be challenging to achieve, the appliance will have bite blocks, screws and connectors for both jaws to position the lower jaw in the desired position,” she said.
Naturally, visits to the dentist are required to “calibrate and adjust how much the lower jaw will be shifted forward”.
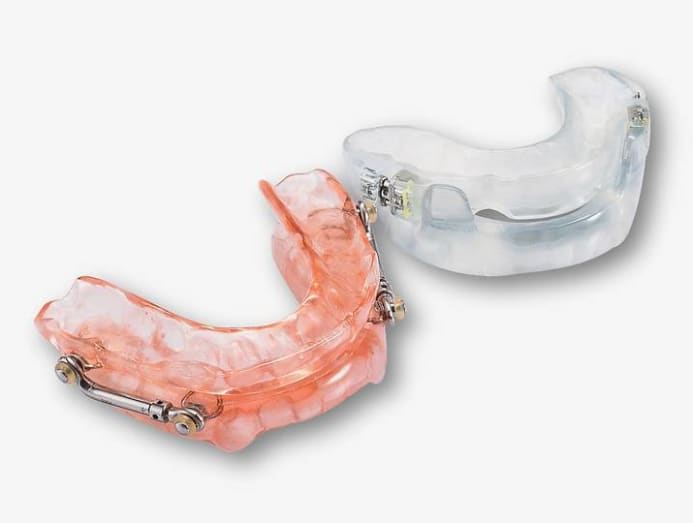
Regular follow-up visits are important, too, as the dentist “will need to check on the patient’s bite and jaw relationship, which may change with time” said Dr Anandarajan. With care and maintenance, the oral appliances can last about three years.
But like the CPAP machine, the oral appliances also have their shortcomings, such as short-term side effects including excessive salivation, mouth dryness, difficulty in chewing, tooth pain, gum irritation, headaches, and jaw discomfort, said Dr Tan.
In the long run, the oral appliance could elicit dental and bite changes. “It is therefore advisable that oral appliances be dispensed and fitted only by dental specialists who treat sleep-related breathing disorders,” said Dr Tan.





