Infant eczema: Genes play a role but symptoms can be controlled, doctors say
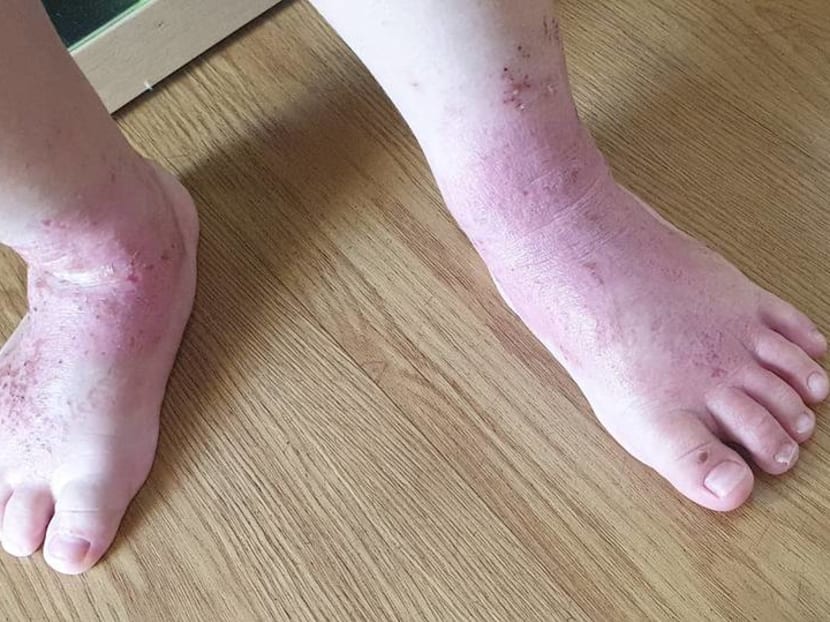
Ms Serene Koh's son was diagnosed with eczema when he was just a few months old. (Photo: Serene Koh)
SINGAPORE: Patches of scaly, cracked and inflamed skin on tiny feet. Blood on clothes. Painful screams during shower time. Sleepless nights.
Ms Serene Koh’s son was diagnosed with eczema when he was just a few months old. When he started getting itchy rashes on his skin, she took him to a hospital where he was diagnosed with the skin condition.
He would scratch his skin until it bled, she said.
“It was very heartbreaking to see because as a baby, he could only cry, (he) couldn’t verbalise the pain that he was going through,” said Ms Koh, who also suffered from eczema when she was younger.
It was a “struggle”, said the 37-year-old social worker, adding that she had many sleepless nights over her son's condition.
READ: Tackling that itch: Demand for help with skin issues on the rise in Singapore
A prick test found that he was allergic to peanuts, so Ms Koh, who was breastfeeding her son, cut that out completely from her diet.
“It seemed to show some improvement, but it was still not better. They (doctors) gave creams to apply, which had steroid in them,” she said.
“It would get better, then it would come back, get better, then come back.”
He hated taking showers.
“Every time he took a shower, he would scream. Because after he scratched, the skin would be open and red,” said Ms Koh.
His itch also seemed worse at night, keeping him and the family up.
“I would help him to scratch, not using my nails, but just to help him with it because I know that if I helped him to scratch, I won’t tear his skin.”
Ms Koh tried multiple things to ease her son's discomfort: Probiotics and fish oil, traditional Chinese medicine, and a mositurising regime.
She also brought her son to a dermatologist and covered his feet with socks, but he would pull them off.
His feet remained itchy.
“The doctors advised us to wrap his feet up so he cannot scratch it. Because in order for the skin to heal, he has to stop scratching and scratching is a habit,” she said.
Pants with enclosed covering for the feet came to the rescue.
Ms Koh also avoided situations that would make him perspire.
“Heat will make it worse, so we couldn’t bring him outdoors as much. So ideally, and for the most part, we just spend (time) in aircon and indoors because we noticed that sweat would make it worse and he would scratch,” she said.
Her son is now three years old and his condition is under control, she said.
“There is hope. There’s really hope, because having gone through it, I feel a lot for mums who are also going through it and feel like there’s no end in sight,” she said.
Commentary: Low self-esteem, depression and frequent flare-ups plague growing numbers of eczema sufferers
PREVALENCE OF ECZEMA AMONG CHILDREN
Ms Koh’s son is not alone in his fight against the skin condition. Doctors CNA spoke to said they have seen an increase in the number of children getting diagnosed with eczema.
The prevalence of eczema- also known as atopic dermatitis - is around 30 per cent in babies under the age of one, said Dr Elizabeth Tham, head of the division of Paediatric Allergy, Immunology & Rheumatology, at the Khoo Teck Puat – National University Children’s Medical Institute.
Among older children, this percentage is 20 per cent, she said.
“There is an increasing number of children with moderate and severe atopic dermatitis, and these patients make up about 20 to 30 per cent of the eczema patients treated at the KKH Dermatology Service,” said Associate Professor Mark Koh, who heads the service.
“There appears to be a general increase in trend on the incidence or prevalence of atopic eczema in children over time. In my practice I do see more infants with eczema,” said Dr Lee Bee Wah, a paediatrician at The Child and Allergy Clinic at Mount Elizabeth Medical Centre.
Dr Tan Hiok Hee, senior consultant dermatologist at Thomson Specialist Skin Centre, similarly noted this increase.
He attributed the rise to an “overall increase in prevalence of the condition” and also more awareness of the condition.
“Parents thus are more likely bring in their kids for a review and diagnosis when they note their children having recurrent itchy rashes, instead of self-medicating,” he said.
WHY DO CHILDREN GET ECZEMA?
Doctors said that eczema are caused by genetic factors, but that there are other factors that may aggravate the condition.
"Children affected may have a history of other sensitive disorders such as asthma and rhinitis, and there is often a family history of similar conditions," Dr Tan said.
Besides genetic factors, the high prevalence of eczema in Singapore is similar to that observed in other developed countries, "suggesting that environmental factors may be important in determining the expression of the disease", he said.
Dr Tham, whose patients include infants and children up to 18 years of age, said that the most common reason for eczema is a genetic predisposition, or a strong family history of allergic diseases.
“This results in excessive skin dryness even from birth, and in some patients, there may be a genetic defect in a skin barrier protein called filaggrin which is responsible for maintaining an intact skin barrier,” she said.
Assoc Prof Koh, who cited similar reasons, said that beyond the genetic basis of eczema, environmental factors “play a role in triggering or worsening atopic eczema”.
He pointed to dusty environments, pets, carpets, stuffed toys, smoking, strong soaps and detergents, and insect bites as some of these environmental triggers.
Emotional stressors such as exams can also trigger eczema, Assoc Prof Koh said.
Atopic eczema, however, is a complex condition, Dr Lee said.
“It is difficult to pinpoint the reasons. The main issues in eczema is a weakened skin barrier and abnormal regulation of the immune system that tends to promote inflammation,” she said.
Doctors said that the onset of the condition for most patients begins before they turn one, although some children may only develop symptoms later in childhood or during their teenage years. The condition may persist into later in their lives, they said.
While the condition cannot be prevented and there is currently no known cure, the symptoms can be controlled, doctors said.
WHAT CAN PARENTS DO TO HELP THEIR CHILDREN?
“With the use of gentle soaps or soap substitutes and daily moisturisers from infancy, the onset of eczema can be delayed, and the severity of eczema can be reduced,” said Assoc Prof Koh.
Early treatment once the symptoms occur is also important to prevent the worsening of the condition, he added.
Assoc Prof Koh, who said that food allergies have increasingly been found to worsen the condition in infants, also said that reducing triggers can also help prevent the condition from worsening.
While doctors encourage young patients with eczema to maintain a healthy lifestyle including participating in outdoor activities, there are some situations that are best avoided, he said.
“When the weather gets too warm, hazy, or when your child has an eczema flare, it is best to limit such activities and increase the frequency of moisturiser applications to reduce the skin inflammation,” he said.
Dr Tan said that aggravating factors include exposure to sudden changes in room temperature and certain types of clothing material such as wool.
“Many children with atopic eczema are sensitive to house dust mite, so I usually advise reducing the amount of carpeting and soft toys which tend to trap a lot of the mites,” he added.
In older children, stress and their emotional state can also aggravate eczema, he said.
“It is also important to explain to the child that it is not their fault that they have eczema, and to look into the psychological aspects of eczema as well. Some of these children may be teased or shunned by their peers, and may develop a negative self-image,” he said.
Dr Lee said that skin care is important in the management of eczema. Dr Tham said that a multi-pronged approach including applying moisturisers to keep the skin hydrated, treating concurrent skin infections with antibiotics and applying topical steroids to control inflammation help prevent the condition from worsening.
COMMON MYTHS
Although topical steroids are “essential treatment modalities to control inflammation”, Dr Tham said that one of the myths about eczema is that using steroids will make the child “dependent” on them or that avoiding steroids will help the child outgrow eczema faster.
“Without adequate control of the inflammation, the eczema can become worse and lead to complications,” she said.
These complications include infections, bleeding, and food allergies due to food allergens entering the skin, she said.
“Proper treatment with topical steroids and moisturising will help control the eczema well, and the child will then be more likely to outgrow the condition. If the eczema is uncontrolled, the chances of outgrowing it will be much lower,” she said.
Dr Lee said that an important misconception that eczema is caused by allergies.
“In fact, the scientific evidence points the other way round - that eczema predisposes to food allergy,” she said.
Among other myths surrounding the condition is that eczema is due to poor hygiene, or the mother taking excessive amounts of seafood during pregnancy, said Dr Tan. Some think that it is infectious and can be passed to others through touch or contact, which is also a myth, he said.
“Some people believe that eczema is due to a ‘weak’ immune system and need to further boost their immunity – this is not true,” he added.
Despite the difficulties children and parents face with the condition, there may be light at the end of the tunnel.
A “big proportion” of mild infant eczema “does remit” as the child grows older, Dr Lee said.
“The good news is that although the sensitive skin will remain with the child into his teenage years and in some cases, beyond, the eczema does tend to get better and gradually improve in most cases,” Dr Tan said.






