She got her master’s degree and raised four children, even as she battled a painful, incurable skin disease
Shortly after her wedding and newly pregnant, Yuzlina Yaacob developed pus-filled blisters all over her body. She shares with CNA Women the struggles of living with generalised pustular psoriasis, a painful lifelong autoimmune disease that affects the skin, and how she went on to have several children and get a master’s degree.

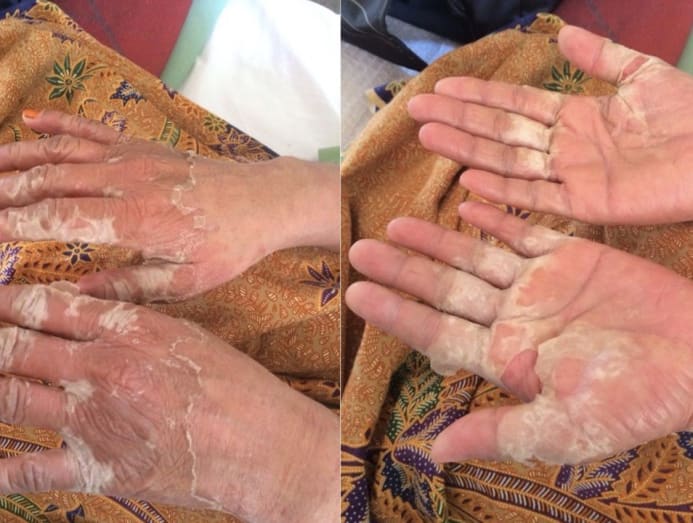
Diagnosed with a painful and incurable skin disease which worsens during pregnancy, Yuzlina Yaacob overcame great trials to have four children. (Photo: Yuzlina Yaacob)
Yuzlina Yaacob always knew she wanted a large family. At the age of 26, she got married, and a month later, became pregnant. Two months into her pregnancy, in October 2005, Yuzlina discovered she had generalised pustular psoriasis (GPP), a rare, incurable skin disease that’s also an autoimmune disorder.
Her generalised pustular psoriasis symptoms first appeared as painful pus-filled blisters on Yuzlina’s right thigh, covering an area 4cm in diameter. Then, another patch appeared on her right hand.
“It was the first year of my marriage, so I felt too shy and embarrassed to tell my husband. I locked the door of my room and tried to settle it myself,” said the Malaysian, who now lives in Kelantan.
They looked like pimples to Yuzlina, so she broke the pustules with a needle, releasing a foul-smelling pus. She then applied traditional Malay ointment over the area.
However, the pustules came back a few days later, and were bigger and more painful.
Yuzlina decided to tell her husband and she also sought treatment at a hospital in Johor Bahru, where she was living then.
I had to cover my bed with a big blanket at night so that the pus wouldn’t stain the bedsheet. It was so itchy and painful that I cried all the time.
She was diagnosed with generalised pustular psoriasis, a severe non-contagious skin disorder where abnormal inflammation causes pustules to develop over large areas of the body. It may be exacerbated by pregnancy in some cases.
Worried that oral medication would affect her unborn baby, her doctor prescribed only topical medication such as medicated shampoos and creams.
Yuzlina’s condition rapidly deteriorated as her pregnancy progressed. Soon, pustules covered her entire body, including her face, scalp, ears and even the inside of her nose.

“My whole body was like a corn cob covered with kernels, and filled with pus. I had to cover my bed with a big blanket at night so that the pus wouldn’t stain the bedsheet. It was so itchy and painful that I cried all the time,” she said.
UNDERSTANDING GENERALISED PUSTULAR PSORIASIS
WHAT IT IS
The rarest form of psoriasis, an autoimmune disorder. In GPP, large areas of the skin become red, and develop itchy and painful pus-filled blisters known as pustules. It is not contagious.
SYMPTOMS
These pustules may flare suddenly, last for a few weeks and then clear up partially or completely on their own. Patients sometimes also develop a fever, shivers, headaches, a rapid pulse, muscle weakness, nausea, fatigue and joint pain.
WHAT CAUSES IT
It has been linked to genetic mutations, and can be triggered by steroid withdrawal, infections, stress or pregnancy. It usually affects adults, though children can get it as well.
TREATMENT
This is an incurable condition. However, doctors may prescribe topical medication, oral medication and phototherapy to control symptoms. Pregnant women will also be monitored more closely to ensure the safety of mother and foetus.
The information is taken from the National Psoriasis Foundation in the US and DermNet, a dermatology resource in New Zealand.
A TRIAL FOR THE NEWLYWEDS
After her diagnosis, she felt she was unable to continue working and resigned from her job as a marketing executive. Things worsened from the third month of pregnancy, when she became bedridden.
Her husband, now the sole breadwinner of the family, would serve her food in bed. He also took over the household chores.
“I told him to wash my clothes separately from his. But he said, there is no need, because (GPP) is not contagious. He washed all our clothes together,” she said.
Yuzlina’s husband even bathed her. “He brought a pail of water and helped me wash my hair while I lay in bed. He did not feel afraid of me or awkward while doing this,” she said.
SURVIVING PREGNANCY AND MOTHERHOOD
Pregnancy became even more challenging with GPP.
Yuzlina missed many antenatal checkups. When she did go for a checkup, she went in a wheelchair. “I couldn’t walk because there were pustules under my feet. I also couldn’t wear shoes and just wore slippers.
“(My skin condition) was so bad that I thought I would die,” she said.
“When I arrived for my appointment, the nurses or doctors would be shocked and afraid when they saw my condition. They would ask what happened. So I had to tell them the same story again and again,” she said.
Yuzlina delivered her baby at seven months gestation, possibly due to the stressful pregnancy, she said. The infant weighed 2kg.
The disease continued to overshadow the joys of new motherhood.
“After giving birth, it was heartbreaking that I could not carry my baby because pustules covered my arms. I breastfed her by putting her on the bed and moving my body towards her,” she recalled.
COPING WITH THE PAINFUL SKIN CONDITION
After delivery, Yuzlina started on oral medication and her condition improved within two months. The pustules became smaller and were isolated to certain parts of her body.
She learnt to live with GPP, and in 2007, enrolled in a full-time master’s degree in human resources at Universiti Teknologi Malaysia (UTM) in Johor Bahru. Shortly after enrolling, she discovered she was pregnant again.
“I was shocked and worried that a big wave of psoriasis would come again. I wondered how I was going to study, and cope with pregnancy, a new baby and psoriasis,” she said.

Sure enough, her pregnancy exacerbated her disease. She had stopped her oral medication and pustules covered her whole body, although this time, they did not appear on her face.
“It was crazy. Under my clothes, I had a lot of itchy, painful pustules that nobody knew of. I walked like a penguin because pustules covered my legs. When I sat down, the pustules sometimes broke and stained my clothes,” she said, adding that she would wear dark clothes to class.
Nonetheless, Yuzlina carried her pregnancy to full-time and gave birth to a healthy baby boy in February 2008. Two weeks later, she returned to her classes and completed her degree.
BUILDING A BIGGER FAMILY
By now, Yuzlina knew pregnancy was a big trigger for GPP. But it didn’t stop her from hoping for more kids.
“I have always wanted to have a big family. So I told myself I would overcome these challenges and get stronger,” she said.
In 2010, she gave birth to another daughter and also returned to the workforce, teaching at UTM.
Sadly, a year later, during a family holiday in Indonesia, the child fell down from a height of 10 steps, and passed away.
The unimaginable grief caused Yuzlina’s psoriasis to flare. “My whole body became covered with pustules and I couldn’t walk. I wanted to go to her grave to see her for the last time before she was buried, but I just couldn’t go,” she said, welling up with tears.
It took Yuzlina a long time to come to terms with her loss. But in 2015, she delivered a pair of twin girls.

Then, in February 2019 at the age of 40, she became pregnant with twins again, but miscarried within four to five months.
When she became pregnant again in September that year, her doctor advised her to terminate the pregnancy. He said that her skin disease, the medication she had been taking and her previous miscarriage might affect the baby’s development and take a huge toll on her health.
After a painful discussion with her family, Yuzlina heeded her doctor’s advice. She also had a bilateral tubal ligation procedure to block her fallopian tubes and prevent future pregnancies.
FAMILY IS EVERYTHING
Yuzlina, now 44, works part-time as a real estate agent. Her four children are now 17, 15, and eight. While she has learned to cope with generalised pustular psoriasis, she told CNA Women that it is often a lonely journey.

She said her condition worsens whenever she gets angry, upset or stressed, or when the weather is hot, so she is often unable to join social activities such as weddings.
“Even though I am usually strong and positive, there are times when I feel down and just want to isolate myself,” she added.
“Sometimes, when I have flares, and the younger kids want to hug me, sit near me, or touch my arms or back, I will tell them not to come close to me. I am afraid my pustules will break,” she said.
The love, acceptance and understanding of her family has been vital in getting her through tough times, she said.
“When I have flares, I gather my kids and ask them to help me apply cream. They all want to help, and don’t feel disgusted or annoyed. They would even kiss my pustules and touch them gently. Even though I am sick, I feel better because of their care for me,” she said.
“Generalised pustular psoriasis is unpredictable – it can get better or worse. I have come to accept it. What is most important is family support,” she said.
Read this story in Bahasa Melayu.
CNA Women is a section on CNA Lifestyle that seeks to inform, empower and inspire the modern woman. If you have women-related news, issues and ideas to share with us, email CNAWomen [at] mediacorp.com.sg (CNAWomen[at]mediacorp[dot]com[dot]sg).







