A first-time mum didn't know she had this risky pregnancy condition until after she gave birth
When Samantha Vinnie Lau was pregnant with her first child in 2020, she didn't know much about preeclampsia. She reveals how the condition went undetected during her pregnancy – and why women should be more aware of it. As told to CNA Women's Sharon Salim.

Samantha Vinnie Lau only knew she had preeclampsia after she gave birth to her daughter on Dec 12, 2020. (Photo: Samantha Vinnie Lau)
I started having swollen feet early in my second trimester. It was only week 15 of my pregnancy, when it became apparent that my feet were swelling, although it was on the mild side.
I understood that swollen feet, also known as edema (swelling caused by fluid retention), is commonly experienced in the third trimester. A friend who was pregnant at the same time told me that it was a bit early in my pregnancy for my feet to swell.
My sister, too, was worried. She said my hands were also swollen, although I couldn’t tell.
BEING UNSURE OF PREECLAMPSIA
My sister and I started googling the cause. She found the term “preeclampsia” and asked me if that could be it.
I started reading up, too, and a lot of articles did, indeed, link feet swelling to a condition called preeclampsia – a serious complication related to high blood pressure during pregnancy.
But although swelling of the ankles and feet were obvious signs, the most telling one was protein in the urine (which is why every pregnancy visit to the gynaecologist includes a urine test).
The thing is, I’d always passed my urine protein dipstick tests. At my pregnancy follow-ups, although several of my blood pressure readings were on the higher side of the spectrum, a second reading (after resting) always produced an acceptable result.
My doctor didn’t think it was preeclampsia as I’d only experienced swelling, and those with the condition would need to have two out of these three symptoms to be diagnosed:
- Protein in the urine (which wasn’t detected in my urine tests)
- High blood pressure (which was at times borderline in my case but wasn’t a cause for worry)
- Swelling of the hands or feet
WHAT TO KNOW ABOUT PREECLAMPSIA
What it is: Preeclampsia is a pregnancy complication characterised by high blood pressure and signs of damage to another organ system, most often the liver and kidneys, said US non-profit academic medical centre Mayo Clinic.
Mothers should be aware of preeclampsia, which can appear very late in the pregnancy, warned Dr Koh Gim Hwee, a specialist and consultant in the Obstetrics & Gynaecology Department at Raffles Women’s Centre.
How it’s diagnosed: “A major sign includes blood pressure that remains above 140/90 and does not come down,” said Dr Koh.
Preeclampsia can be prevented, if mothers take care of the pregnancy well from the early second trimester – when the placenta (the organ which transports oxygen and food to the baby) is still developing. If the early formation of placenta is not adequate, as it expands, some areas will not receive adequate oxygenation, he added.
Incidence rates in Singapore: It’s about 4 per cent of pregnancies seen at KK Women’s and Children’s Hospital, said Professor Tan Kok Hian, Head and Senior Consultant, Perinatal Audit and Epidemiology Unit, Division of Obstetrics and Gynaecology at KKH.
Global preeclampsia rates range from 3 to 8 per cent of pregnancies – although Prof Tan added that with better management of the condition over the years, the rate of complications from preeclampsia, such as eclampsia (convulsions from severe preeclampsia), has dropped significantly.
When it can be life-threatening: It can be deadly if the mother develops eclampsia – in Nov last year, 27-year-old local singer Nadya Dean fell into a coma after giving birth to her second baby, and died 16 days later.
“Preeclampsia is related to the placental small vessels. For certain reasons, if the placental blood vessels are not good, the blood flow that goes through it would have a tendency to form clots which, in turn, could damage the placenta,” explained Dr Koh.
Poor blood circulation in the placenta leads to poor foetal growth, he added, and the clotting in small vessels can also happen in the kidneys, leading to excess protein in the urine.
Treatment and management: To treat preeclampsia, your obstetrician will have to decide whether you should be delivered earlier, said Dr Koh. A woman would recover once she delivers the baby (and the placenta). It is important to have her blood pressure back to normal before she's discharged.
To reduce the occurrence of preeclampsia, a patient who is at high risk may often be prescribed aspirin and, from early in the second trimester, an increase in calcium tablets, Dr Koh told CNA Women.
ENTERING HER THIRD TRIMESTER: ‘NOTHING HELPED’
Going into my third trimester, in late Oct 2020, the swelling was so bad that I had to buy new shoes. It was also the month I had to return to the office – I work in the events industry, and physical events had resumed.
While I was thankful that I got to move about more, it was also painful to walk around with swollen feet.
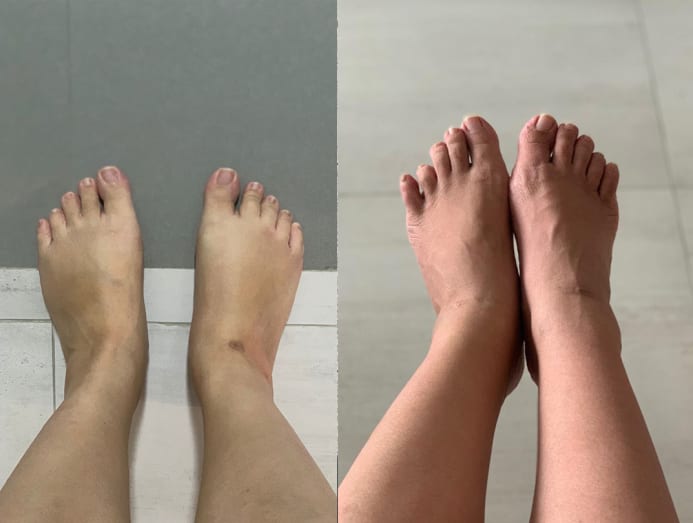
Everyone was saying I had “elephant feet”.
My doctor also advised me to buy compression stockings (meant to reduce discomfort and swelling). But my feet, ankles, calves and legs were so swollen that it was almost impossible for me to put them on. I also wasn’t able to stand, walk and sit as the compression stockings were very tight.
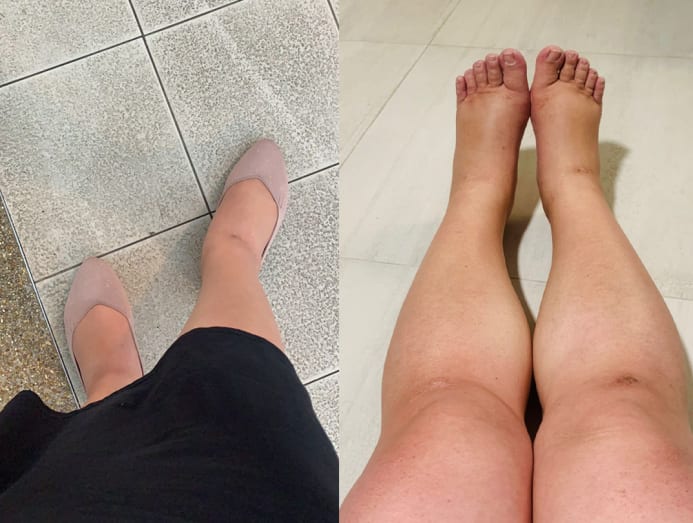
The doctor also told me to try elevating my feet to reduce the swelling; my husband even got me to watch my diet. I even tried soaking my feet into both cold and hot water.
But nothing helped. There was perhaps only a 20 per cent reduction in the level of discomfort, but not the swelling. Everyone was saying I had “elephant feet”.
I enjoy cooking, and would cook for myself when I was pregnant. But I couldn’t stand for more than 30 minutes in the kitchen, and it was uncomfortable. It felt like your skin was being stretched.
At the back of my mind, I still didn’t think it might be preeclampsia. I just thought I was a unique case and tried to live with it. There were support groups where fellow mums shared that they had swollen feet but did not have preeclampsia.
GIVING BIRTH: ‘A SUDDEN SPIKE IN MY BLOOD PRESSURE’
My final appointment with my gynaecologist was on Dec 11, four days before my estimated delivery date of Dec 15.
But during the visit, because of a sudden spike in my blood pressure – it was 160/114 (a normal reading is 120/80) – my doctor said she couldn’t let me go home for my safety.
A major sign includes blood pressure that remains above 140/90 and does not come down.
I was asked to remain in the clinic, where the staff would monitor my blood pressure. They brought me to a room to rest and strapped me to a blood pressure monitor. Within the first hour, they had checked my blood pressure three times. They must have taken readings at least six times over approximately three hours.
My doctor told me that should the readings still be high, I would have to be admitted to hospital that day and induced for delivery. She also explained that due to the consistently high blood pressure, I might faint or experience seizures.
My blood pressure remained consistently high, with the highest being 182/120. The readings were off the charts.
The nurses even took out a traditional blood pressure machine (in case the digital machine was not working), and I still “failed”. They were very concerned too.

I was admitted to hospital that day, and had a vaginal tablet inserted to induce labour. At 6.30pm, I felt waves of pain, and a nurse told me that they were contractions.
By 10.30pm however, there was still no sign that my cervix was dilated. The doctor told me that I’d move to the labour ward at midnight, where I would have a second tablet inserted.
I experienced mild contractions through the night but when my doctor arrived at 9am the next day, she said the contractions were reducing. Did I want to take a third pill or go ahead with a Caesarean delivery, she asked.
I decided to take the third tablet, as I wanted my husband to witness the birth of our first child.
By 5pm, I was in a lot of pain but my cervix was still not dilated. It was time for an emergency Caesarean section – I wasn’t only trembling from the pain, the baby’s head was not engaged at all.
Half an hour later, my baby girl was born, safely and healthily.
FINDING OUT IT WAS PREECLAMPSIA: ‘IT WAS SHOCKING’
At the time that I was admitted to the hospital, my gynae asked for further tests to be done as she, too, was concerned about my suddenly high blood pressure. So my blood was tested and my urine was collected over the course of 24 hours.
I also didn’t expect that preeclampsia could be discovered that late in pregnancy. I thought that if you have it, you would know it early.
When she visited me the morning after my delivery, she said that protein had been detected in my urine, confirming that I had preeclampsia.
When I found out, I had many questions: Why wasn’t it discovered earlier? Technically, I could have died, and other complications could have happened.
I was shocked that the urine stick that every pregnant woman relies on – which shows if you have protein in your urine – could be inaccurate. It was only after they’d collected my urine over 24 hours that the results showed protein was present.
I learnt that preeclampsia doesn’t only affect women during pregnancy, but also after giving birth. Following my delivery, I had to check my blood pressure two to three times a day. Thankfully, after about three weeks, the readings came down and everything went back to normal.
To reduce the occurrence of preeclampsia, a patient who is at high risk may often be prescribed aspirin tablets and, from the early second trimester, an increase in calcium tablets.
At my postpartum review, my doctor told me I would have to take aspirin during future pregnancies, to thin the blood and manage preeclampsia. I reckon that I’d need to take my blood pressure regularly on my own as well, just to be safe, as I am at a higher risk for preeclampsia.
MORE AWARENESS NEEDED ABOUT PREECLAMPSIA
Looking back, I realise that many women hadn’t heard of preeclampsia, and no one talks about it until it happens to them.
When I found out, I had many questions: Why wasn’t it discovered earlier? Technically, I could have died, and other complications could have happened.
Very recently, a girlfriend who gave birth reached out to ask about my experience with preeclampsia. She hadn't been officially diagnosed with it but her blood pressure was quite high and there was protein in her urine. I remember her saying she had swollen feet, too. Perhaps her case was undetected too.
I also didn’t expect that preeclampsia could be discovered that late in pregnancy. I thought that if you have it, you would know it early. I also thought it was a pre-existing condition.
So when I discovered only after I gave birth that I had preeclampsia during pregnancy, I was shell-shocked. I remember that at the time that my feet started to swell, I came across YouTube videos of women who had died from preeclampsia. But I brushed off the fear, not wanting to scare myself.

Pregnant mothers should be equipped with knowledge about preeclampsia. It’s something that should be brought up early and talked about more. Family members should be educated as well. My husband hadn't heard of the condition either, and it didn’t occur to him that it was serious.
If the couple is concerned about it, they should not dismiss it but bring it up to their doctor – even if the woman is only experiencing one symptom.
CNA Women is a section on CNA Lifestyle that seeks to inform, empower and inspire the modern woman. If you have women-related news, issues and ideas to share with us, email CNAWomen [at] mediacorp.com.sg (CNAWomen[at]mediacorp[dot]com[dot]sg).










