Mammogram, HPV test, pelvic ultrasound: What happens at each one and how can women prepare for them?
How often should you do such health checks? When is the best time of the month to do them? How much discomfort is involved? CNA Women takes a deep dive into the important health checks – for the breasts and reproductive system – that every woman should do.

Medical professionals give insights on the important health checks women should do, including discomfort level, the best time of the month to do each one, and any pre-test prep you need to do. (Photo: iStock/AsiaVision)
Perhaps it’s an age thing but gone are the days where my girlfriends and I talk about the hottest actor or the newest IT bag. These days, the conversations among my 30-something and over 40-year-old girlfriends revolve around our body aches, bouts of insomnia and of course, the increasing number of health checks we need to do.
Just the other day, one of my girlfriends was regaling us with tales of her first mammogram. “There’s just so much squeezing involved. And just when you think the metal plates can’t squeeze your boob anymore, they squeeze it some more!”
Which made me wonder, why are these health checks necessary and how often do we really need to get them done? Is it fine if we skip a year or two? Plus, why do some of these tests have to be so uncomfortable?
The discomfort was one of the issues discussed on the new CNA Women podcast Womankind. Pap smears, the Human Papillomavirus test, mammograms and internal ultrasounds are important to a woman's health, yet they can be so anxiety-inducing that we delay getting them. What are the ways that women can reduce the stress of having to undergo them?
Listen to the full Womankind episode here:
If you’re still tempted to put any off – just one more year, we can hear you – remember the breast cancer slogan: Early detection saves lives. And it’s not just for your breasts.
Get the lowdown on the different tests that women need, the discomfort level, if any, and everything else you need to bear in mind for each test, below.
HOW TO CARE FOR YOUR BREASTS
Breast cancer is the most common cancer among women in Singapore, affecting one in every 13 women here.
According to the 2020 Singapore Cancer Registry Annual Report, every year, about 2,165 women are newly diagnosed with breast cancer, with about 436 dying from the disease.
Just having breasts puts one at risk. “You do not need to have a family history of breast cancer or cancer of any form to be at risk of developing breast cancer,” said Dr Lee Wai Peng, senior consultant and breast surgeon at Solis Breast Care and Surgery Centre.

Currently, the most effective way to detect breast cancer at an early and treatable phase is with a mammogram screening.
However, a mammogram is only suitable for women aged 40 and above. “Younger women have denser breasts, which may make the mammograms less sensitive to picking up small cancers,” Dr Lim Siew Kuan, senior consultant and breast surgeon at Solis Breast Care and Surgery Centre, explained.
However, Dr Lim does add that for women with high risk factors, such as hereditary genetic mutations, personal history or a strong family history of breast or ovarian cancer, bi-annual or annual breast screenings might be recommended much earlier. In such instances, it would be best to consult your doctor for a screening schedule.
But that’s not to say that women under 40 need not do any breast care. Make sure to do your monthly breast self-examination (BSE). Dr Lim said most women frequently forget to do so, and regular BSE can help them pick up any changes that might occur. It’s also interesting to note that BSEs need to be done continually throughout your life.

“Women above the age of 18 should do their BSE once a month, between day seven and day 10 of their menstrual cycle. This is the period when the breasts feel the least lumpy, and any recent breast change can be picked up,” Dr Lim explained.
But if your menses is irregular, or if you’re post-menopausal, Dr Lim advised choosing a fixed day of the month to do your BSE.
Your doctor might also get you to do a breast ultrasound. Even so, while a breast ultrasound can detect abnormalities in the breast tissue, Dr Lim said it should not replace your annual mammogram.
This is because a breast ultrasound is usually done in tandem with a mammogram, to add information where needed, or to help guide the placement of needles for procedures such as a biopsy.
“The mammogram and breast ultrasound are useful in picking up different abnormalities. A mammogram can detect abnormal calcifications or architecture distortion, which are the earliest signs of breast cancers … therefore making mammography the gold standard for breast screening in women who are asymptomatic.
“However, if the mammogram reveals dense breasts or any abnormalities, a breast ultrasound can be used as an adjunct to delineate further details in the breast tissue,” said Dr Lim.
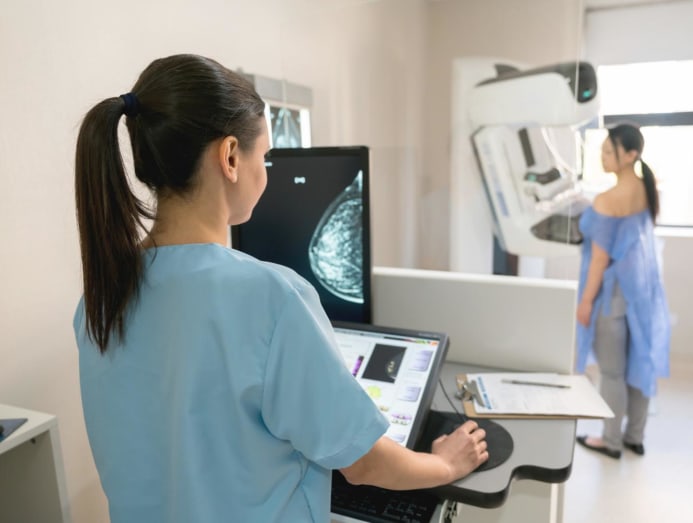
MAMMOGRAM
What to expect: You’ll be brought into a room and asked to stand in front of a special X-ray machine. Here, you’ll be asked to place one breast onto a plastic plate in front of you. Another plate, known as the paddle, is then lowered from above. The plates compress the breast, holding it still for the X-ray to be taken. This lasts for a few seconds. The process is repeated for a sideward view of the breast, and then for your other breast.
According to Dr Lee, the compression or spreading out of the breast in this way allows for a “better view of the breast and to detect normalities”.
How often should you get checked: Normal-risk women aged 40-49 years may choose to do a yearly mammogram but should speak to their doctor about the pros and cons of screening, taking their risk profile into account. Women above 50 should do a mammogram every two years
Best time to get checked: Book your appointment for at least one week after the start of your menses, as your breasts will be less tender and sensitive.
Comfort level: Many women do find the compression to be uncomfortable, sometimes even painful. “If you encounter severe pain during the compression, do inform the radiographer as slight adjustment of the breast may help to relieve this discomfort,” said Dr Lee.
Pre-appointment prep: Avoid using perfume, deodorant, powder or ointment around the breasts and armpits as they can affect the test results.
BREAST ULTRASOUND
What to expect: A much more comfortable test compared to the mammogram as it’s done with you lying down. Your doctor or a sonographer will place a gel-coated transducer probe on your breast and look for any lumps or abnormalities within.
In order to examine the tissues and structures of your breast, photographs of your breasts will be taken at different sites and from various angles. During this process, you may be asked to hold your breath briefly to facilitate image taking.
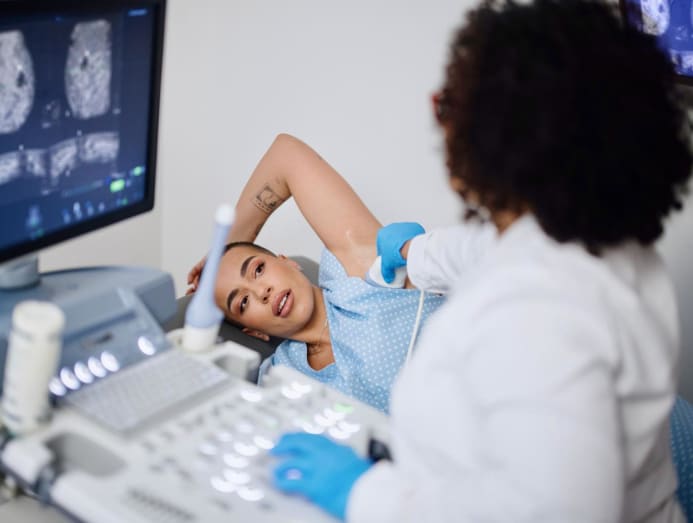
How often should you get checked: Depending on your breast density, you may be encouraged to get a breast ultrasound annually together with your mammogram. But do check with your doctor about whether this is necessary for you, given your own risk factors and health profile.
Best time to get checked: Similar to a mammogram, book your appointment a week after the start of your menses.
Comfort level: Completely comfortable, though you might feel a teeny discomfort if the transducer probe scans over a sensitive or tender area of the breast.
Pre-appointment prep: Similar to-dos as a mammogram.
HOW TO CARE FOR YOUR REPRODUCTIVE SYSTEM
In Singapore, three gynaecological cancers – cervical, ovarian and uterine – are among the top 10 cancers affecting women, with cervical cancer being the most common.
While there is currently no routine screening for women who have no known risk factors for ovarian and uterine cancers, there are two tests that you can take as part of the National Cervical Cancer Screening programme: Pap smear and Human Papillomavirus (HPV) test.
The HPV test looks for the presence of HPV infection, which is the primary cause of cervical cancer, while a Pap smear detects pre-cancerous changes in the cervix.
While Pap smears used to be the standard test for cervical cancer, doctors are now recommending HPV testing as a much more effective method.

Professor Yong Eu Leong, emeritus consultant at the Department of Obstetrics and Gynaecology, National University Hospital Singapore, said the HPV test can be likened to a “PCR test to detect genetic materials from strains of the HPV that may be growing within the cells in the neck of the womb”.
“The HPV test detects the virus that is causing the cancer and the Pap smear detects the cells that has turned cancerous due to the effect of the virus,” he added.
PAP SMEAR OR PAP TEST
What to expect: You will need to remove your underwear and lie on an examination table, with your knees bent. The doctor then gently inserts an instrument known as a speculum – a duck bill-shaped device, that allows him or her to open the walls of your vagina. Then using a soft brush and spatula, the doctor will collect a tissue sample from the cervical wall.
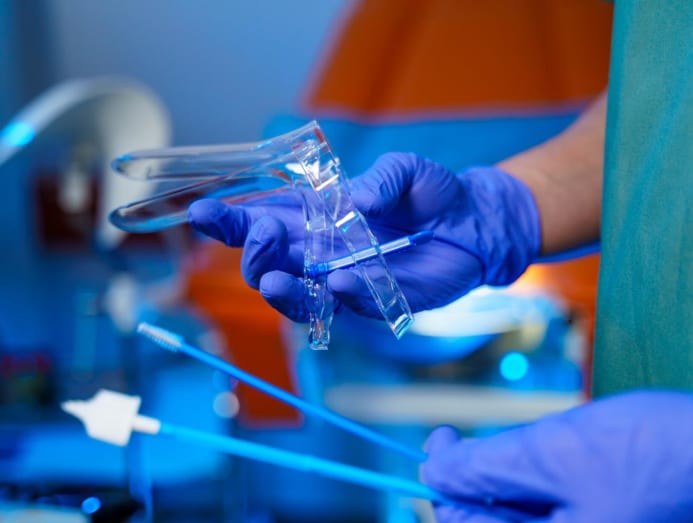
How often should you get checked: Once every three years for women between 25 and 29 years, if you have ever had sex. After 30, women should move on to doing the HPV test.
Best time to get checked: Two weeks after the start of your period, as this allows the doctor to get the clearest and cleanest sample of cervical cells.
Comfort level: Some women do experience a slight discomfort when the cervical cells are being collected.
Pre-appointment prep: Avoid sexual activity and the use of vaginal lubricant, douching products or tampons 48 hours before the test.
HUMAN PAPILLOMA VIRUS (HPV) TEST OR HPV SCREENING
What to expect: The process is similar to getting your Pap smear. In fact, since both the HPV test and Pap smear collect tissue samples from the cervix, both tests are usually performed at the same time, using the same tissue sample.
How often should you get checked: Once every five years for women aged 30 years and above, and yes, this includes even if you’ve been vaccinated against HPV.
Best time to get checked: Similar to a Pap smear. Two weeks after the start of your period.
Comfort level: Similar experience as getting a Pap smear.
Pre-appointment prep: Similar to-dos as a Pap smear.
PELVIC ULTRASOUND SCAN
What to expect: There are two ways to do the scan – via an ultrasound probe inserted into the vagina (transvaginal) or a combination of transvaginal (TV) and transabdominal (TA).
For a TA scan, you’ll lie comfortably on an examination table. Gel is applied over your lower abdomen and the doctor or sonographer presses an ultrasound probe against the skin, moving around to obtain ultrasonic images of the uterus and ovaries.
For a TV scan, you’ll lie on the examination table with your knees bent, and feet and legs supported, like you would during a Pap smear. A lubricated specially-designed probe, usually long and slim (also known as a transvaginal transducer) is then gently inserted into the vagina. The doctor will then turn and angle the probe to examine different areas within.

How often should you get checked: Dr Tan said that women 30 and above may want to consider getting a pelvic ultrasound annually, especially those who are at risk of ovarian cancer. You should speak to your doctor about including a pelvic ultrasound in your routine screening schedule if you have BRCA1 or BRCA2 gene mutations, Lynch syndrome or a strong family history of breast or ovarian cancer in more than one relative.
Dr Tan Toh Lick, obstetrician and gynaecologist from Thomson Surgical Centre, added that a pelvic ultrasound can also help “check for uterine growth, including fibroid, polyp and cancer, as well as ovarian cyst and cancer”.
Best time to get checked: Between days seven and 10 of your menstrual cycle “when the endometrium (uterine lining) is thin and clear, and the ovaries are less likely to have any large follicles, which may be considered to be an ovarian cyst”, said Dr Tan.
Comfort level: Generally, a TA scan is completely comfortable, though you may feel a little uncomfortable with the ultrasound probe pressing firmly against your full bladder (imperative for the doctor to get good images of the area).
For a comfortable TV scan, the key is to remain relaxed, Dr Tan said. Some discomfort is common as the transducer is moved, but the pain should still be bearable.
Pre-appointment prep: A full bladder is required for a TA scan, so you will need to drink at least three cups of water from 30 minutes to an hour before the scan. If you’re getting a TV scan after, you should relieve yourself as an empty bladder is required for this screening.
ONE MORE TEST FOR WOMEN ABOVE 65 YEARS
And while these are the key checks to do, Prof Yong added that another test you might want to include, especially for women above the age of 65, is an “assessment for the risk of menopausal osteoporosis”. This is because not only does bone loss happen naturally with age, women also tend to have smaller, thinner and less dense bones than men.

It involves an osteoporosis screening with your doctor, which includes a physical examination.
You may also be asked to go for a Bone Mineral Density test to measure the mineral content, like calcium, in your bones. Also called Dual Energy X-Ray Absorbitary (DEXA) or bone densitometry, it is an enhanced form of X-ray to measure bone loss, says the Radiology Info website.
According to the Singapore Health Hub website, DEXA detects the amount of energy that has been emitted after the X-ray is done. As bone mass will naturally obstruct the energy passing through, the more energy emitted, the weaker the bone is.
WHERE WOMEN CAN GET TESTED
There is really no excuse for not scheduling your health checks as these are widely available across Singapore, and can be “arranged by doctors in polyclinics, in general practice and in hospitals”, said Prof Yong.
And to make it even easier, you can also check out the national Screen for Life programmes. The Screen for Life – Breast Cancer Screening Programme offers subsidised mammograms from S$50 at participating polyclinics, while the Screen for Life – National Cervical Cancer Screening Programme offers subsidised rates for Pap smears and HPV tests, from S$15 at all polyclinics.
CNA Women is a section on CNA Lifestyle that seeks to inform, empower and inspire the modern woman. If you have women-related news, issues and ideas to share with us, email CNAWomen [at] mediacorp.com.sg (CNAWomen[at]mediacorp[dot]com[dot]sg).